When should you do cardioversion
Cardioversion is usually done to treat people who have atrial fibrillation or atrial flutter. These conditions occur when the electrical signals that normally make your heart beat at a regular rate don’t travel properly through the upper chambers of your heart.
What are the indications for cardioversion?
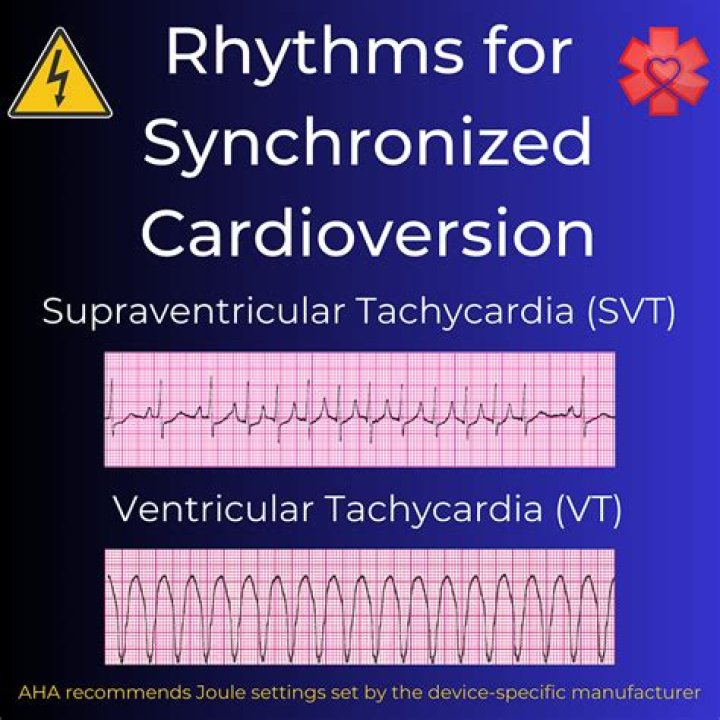
- Supraventricular tachycardia (atrioventricular nodal reentrant tachycardia [AVNRT] and atrioventricular reentrant tachycardia [AVRT])
- Atrial fibrillation.
- Atrial flutter (types I and II)
- Ventricular tachycardia with pulse.
Should I have a cardioversion?
If you have an irregular heartbeat (you might hear it called arrhythmia, atrial fibrillation, or AFib), your doctor will probably suggest a treatment called cardioversion to help you get a normal rhythm back. If your heart beats too fast or unevenly, it can be dangerous.
Who requires immediate cardioversion?
Three types of cardioversion can be used to attempt to change the rhythm of the heart. The initial evaluation for which type to use is the patient’s hemodynamic status. If the patient is hypotensive, has chest pain, altered mental status, or heart failure, immediate electrical cardioversion should be considered.When should cardioversion be delayed?
Early pharmacologic or electrical cardioversion is common practice. However, the wait-and-see strategy, with delayed cardioversion if needed within 48 hours after symptom onset, has several advantages for patients.
Which is better cardioversion or ablation?
Conclusion: In patients with AF, there is a small periprocedural stroke risk with ablation in comparison to cardioversion. However, over longer-term follow-up, ablation is associated with a slightly lower rate of stroke.
Has anyone ever died during cardioversion?
With serial cardioversion 90% of the patients were kept in sinus rhythm for 5 years. Univariate analysis showed that a long duration of arrhythmia and impaired cardiac function were both related to poor outcome. During follow up 3 patients died of progression of heart failure and another 5 died suddenly.
What percentage of Cardioversions are successful?
The success rate of cardioversion with atrial fibrillation is generally better than 90 percent. Chances of success are lower when the atrial fibrillation has been present for more than several months or when the left atrium is very enlarged. In general, there are two ways that a cardioversion procedure for AF can fail.Does your heart stop during cardioversion?
If your doctor recommends cardioversion with medications to restore your heart’s rhythm, you won’t receive electric shocks to your heart. Cardioversion is different from defibrillation, an emergency procedure that’s performed when your heart stops or quivers uselessly.
What happens if cardioversion fails?If external cardioversion fails, then internal cardioversion may be done and involves delivering the jolt of energy through catheters inside the heart. Once you wake up following the electrical cardioversion, you can go home, but will need to have someone drive you.
Article first time published onCan AFib go away?
Paroxysmal atrial fibrillation is one of the types that starts suddenly and goes away own on its own. However, patients should still be monitored and treated. Usually, atrial fibrillation is permanent, and medicines or other nonsurgical treatments can’t restore a completely normal heart rhythm.
Is cardioversion safe for elderly?
Electrical cardioversion can be performed safely in older patients, under sedation and continuous monitoring of blood pressure and oximetry. Available temporary pacing is mandatory to avoid unnecessary bradycardia episodes.
Can AFib be a one time thing?
Types of AFib Episodes can last a few seconds, hours or a few days before stopping and returning to normal sinus rhythm, which is the heart’s normal rhythm. Some people may have single episodes of AFib. However, the condition may progress to the point that it’s constant, which is referred to as chronic AFib.
What is early onset AFIB?
Importance Early-onset atrial fibrillation (AF) can be the initial manifestation of a more serious underlying inherited cardiomyopathy or arrhythmia syndrome. Objective To examine the results of genetic testing for early-onset AF.
How do you treat new-onset AFIB with RVR?
Beta-blockers and calcium channel blockers are first-line agents for rate control in AF. These drugs can be administered either intravenously or orally. They are effective at rest and with exertion. Intravenous diltiazem or metoprolol are commonly used for AF with a rapid ventricular response.
Do you Cardiovert new-onset AFIB?
Cardioversion may be performed electively or emergently to restore sinus rhythm in patients with new-onset AF. Cardioversion is most successful when initiated within 7 days after onset of AF. The need for cardioversion may be acute when AF is responsible for hypotension, heart failure, or angina.
What are the chances of dying from cardioversion?
Results. Electrical cardioversion success rate was 90.4%. Within a year after cardioversion one patient (0.6%) suffered myocardial infarction, three patients (1.9%) had a stroke/transitory ischemic attack (TIA), three patients (1.6%) died and three patients (1.9%) had a bleeding event that required hospitalization.
How long does electrical cardioversion last?
Cardioversion itself takes about 5 minutes. But the whole procedure will likely take about 30 to 45 minutes. That includes time to recover. Abnormal heart rhythms sometimes come back after the treatment.
Who is a candidate for catheter ablation?
An individual who has very bothersome symptoms, such as palpitations, lightheadedness, shortness of breath, and exertional fatigue that is not responsive to at least one concerted effort at antiarrhythmic drug therapy, is a candidate for catheter ablation.
Does metoprolol stop AFib?
It has been shown recently that the beta-blocker metoprolol controlled release/extended release (CR/XL) is also effective in maintaining sinus rhythm after conversion of atrial fibrillation.
How successful is ablation for AFib 2020?
“The success rate of a single procedure for recent onset atrial fibrillation is 70-75%. Compare that to the success rate of 30% with drugs. Even if the patient needs a second ablation, it rises to 80-85%, which is much better.”
Why is a tee done before cardioversion?
The use of TEE may allow cardioversion to be done earlier, may decrease the risk for embolism associated with cardioversion, and may be associated with less clinical instability than conventional therapy.
What does cardioversion feel like?
You may or may not feel a cardioversion shock, but some people describe it as feeling a thump in the chest. You will receive sedatives and pain medications so that you stay comfortable.
What should you not do after cardioversion?
You should not attempt to work, exercise or do anything strenuous until your doctor tells you it is okay to do so. After your cardioversion procedure, your cardiologist or electrophysiologist will make sure that you are taking a blood-thinning medication (anticoagulant) for at least a month in most cases.
Does AFib shorten life expectancy?
Untreated AFib can raise your risk for problems like a heart attack, stroke, and heart failure, which could shorten your life expectancy. But treatments and lifestyle changes can help prevent these problems and manage your risks.
What is the safest blood thinner for AFib?
Non–vitamin K oral anticoagulants (NOACs) are now recommended as the preferred alternative to warfarin for reducing the risk of stroke associated with atrial fibrillation (AFib), according to a focused update to the 2014 American Heart Association/American College of Cardiology/Heart Rhythm Society Guideline for the …
What causes AFib to start?
The basic cause of AFib is disorganized signals that make your heart’s two upper chambers (the atria) squeeze very fast and out of sync. They contract so quickly that the heart walls quiver, or fibrillate. Damage to your heart’s electrical system can cause AFib.
Does pacemaker fix AFib?
Treatment Overview The pacemaker does not treat atrial fibrillation itself. The pacemaker is used to treat a slow heart rate (bradycardia) that happens in some people who have atrial fibrillation.
Should I go to the hospital for atrial fibrillation?
If an AFib episode lasts 24 to 48 hours with no break or if symptoms worsen, call your physician, Armbruster says. Call 911 or go to the emergency room immediately if you experience any symptoms of a stroke, which are sudden weakness or numbness or difficulty speaking or seeing.
What foods are bad for AFib?
- Alcohol. Alcohol tops the list of items to avoid on an atrial fibrillation diet. …
- Caffeine. …
- Grapefruit. …
- Cranberry Juice. …
- Asparagus and Leafy Green Vegetables. …
- Processed and Salty Foods. …
- Gluten.
What is the drug of choice for atrial fibrillation?
Beta blockers and calcium channel blockers are the drugs of choice because they provide rapid rate control. 4,7,12 These drugs are effective in reducing the heart rate at rest and during exercise in patients with atrial fibrillation.



