What pathology is characteristic of osteoarthritis
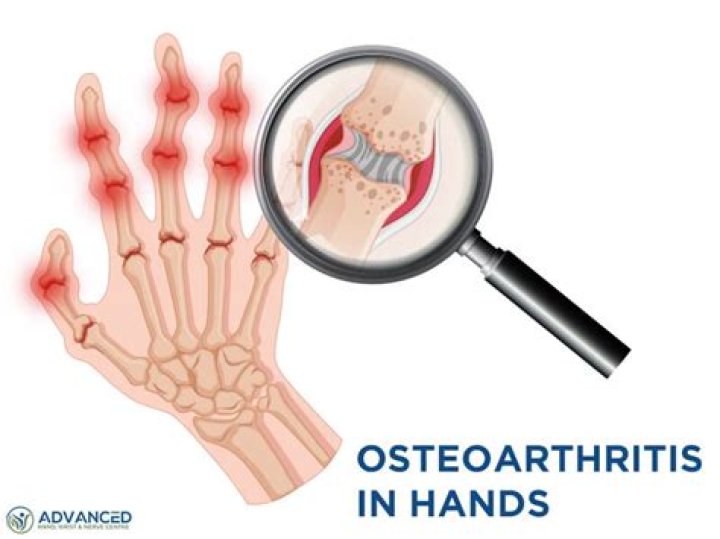
Pathological changes seen in OA joints include progressive loss and destruction of articular cartilage, thickening of the subchondral bone, formation of osteophytes, variable degrees of inflammation of the synovium, degeneration of ligaments and menisci of the knee and hypertrophy of the joint capsule.
What is osteoarthritis give its pathology?
osteoarthritis, also called osteoarthrosis or degenerative joint disease, disorder of the joints characterized by progressive deterioration of the articular cartilage or of the entire joint, including the articular cartilage, the synovium (joint lining), the ligaments, and the subchondral bone (bone beneath the …
What is the most common cause of osteoarthritis?
What causes osteoarthritis? Primary osteoarthritis is caused by the breakdown of cartilage, a rubbery material that eases the friction in your joints. It can happen in any joint but usually affects your fingers, thumbs, spine, hips, knees, or big toes. Osteoarthritis is more common in older people.
How is osteoarthritis characterized?
Osteoarthritis is characterized by the breakdown of joint cartilage. Although it can occur in any joint, usually it affects the hands, knees, hips, or spine. The disease is also known as degenerative arthritis or degenerative joint disease.What pathophysiology means?
Definition of pathophysiology : the physiology of abnormal states specifically : the functional changes that accompany a particular syndrome or disease.
What structures are affected in osteoarthritis?
Osteoarthritis most commonly affects the hands, lower back, neck, and weight-bearing joints such as knees, hips, and feet. Osteoarthritis affects just joints, not internal organs.
Is osteoarthritis a clinical diagnosis?
Because osteoarthritis is primarily a clinical diagnosis, physicians can confidently make the diagnosis based on the history and physical examination.
What's the difference between arthritis and osteoarthritis?
Osteoarthritis is a so-called mechanical condition characterized by the gradual wearing down of cartilage in the joints. Aging is the most common risk factor for osteoarthritis. Arthritis, on the other hand, is not caused by the normal wear and tear of bones.What are the 4 stages of osteoarthritis?
- Stage 1 – Minor. Minor wear-and-tear in the joints. Little to no pain in the affected area.
- Stage 2 – Mild. More noticeable bone spurs. …
- Stage 3 – Moderate. Cartilage in the affected area begins to erode. …
- Stage 4 – Severe. The patient is in a lot of pain.
Age—The risk of developing OA increases with age. Gender—Women are more likely to develop OA than men, especially after age 50. Obesity—Extra weight puts more stress on joints, particularly weight-bearing joints like the hips and knees. This stress increases the risk of OA in that joint.
Article first time published onIs osteoarthritis an autoimmune disease?
Osteoarthritis is not an autoimmune disease, and although the exact causes are not known, multiple risk factors have been identified. In a healthy joint, cartilage provides cushioning and a smooth joint surface for motion.
What causes the degeneration of cartilage?
Cartilage loss caused by a direct injury can result from blunt trauma to the joint. This can be from a severe car accident or even a very bad fall where the joint makes direct impact with the ground. If you’re an athlete, sporting injuries are also a cause of cartilage loss.
What is etiology and pathophysiology?
Definition. The terms “etiology” and “pathogenesis” are closely related to the questions of why and how a certain disease or disorder develops. Models of etiology and pathogenesis therefore try to account for the processes that initiate (etiology) and maintain (pathogenesis) a certain disorder or disease.
What is involved in pathophysiology?
Studies of pathophysiology are concerned with the investigation of biological processes that are directly related to disease processes of physical, mental, or psychophysiological conditions and disorders (e.g., alterations in the endocrine system, in certain neurotransmitters, or inflammatory parameters related to the …
What is included in pathophysiology?
Pathophysiology includes four interrelated topics: etiology, pathogenesis, clinical manifestations, and treatment implications. • Etiology refers to study of the proposed cause or causes of a particular disease process.
What are clinical manifestations of osteoarthritis?
- Pain. Affected joints might hurt during or after movement.
- Stiffness. Joint stiffness might be most noticeable upon awakening or after being inactive.
- Tenderness. …
- Loss of flexibility. …
- Grating sensation. …
- Bone spurs. …
- Swelling.
What laboratory parameters are inherent in osteoarthritis?
Laboratory findings that further differentiate rheumatoid arthritis from osteoarthritis include the following: Systemic inflammation (elevated erythrocyte sedimentation rate [ESR] or C-reactive protein [CRP] level) Positive serologies (rheumatoid factor [RF] or anti–cyclic citrullinated peptide [anti-CCP] antibodies)
Which are common manifestations of osteoarthritis?
The primary symptoms of osteoarthritis (OA) are joint pain, stiffness, and locomotor restriction. Symptoms usually present in just one or a few joints in a middle-aged or older person.
Which part of joint is usually affected by osteoarthritis?
Osteoarthritis primarily affects the weight-bearing joints, that is to say, those of the hip, knee and spine. Some non weight-bearing joints, such as those of the fingers and thumb, can also be affected.
What causes inflammation in osteoarthritis?
However, as osteoarthritis progresses, inflammation can occur around an affected joint. It was thought that the inflammation is caused by cartilage fragments that break off and irritate the synovium (the smooth lining of a joint).
Which element is a risk factor for osteoarthritis OA?
In addition to age and secondary causes such as inflammatory arthritis and prior injury/ trauma, several other risk factors increase the chance of developing osteoarthritis including obesity, diabetes, elevated cholesterol, sex, and genetics. Obesity is a risk factor for osteoarthritis, particularly of the knee.
What is Stage 3 arthritis?
Stage 3 (Moderate) Stage 3 OA is classified as moderate OA. In this stage, the cartilage between bones shows obvious damage, and the space between the bones begins to narrow. People with stage 3 OA of the knee are likely to experience frequent pain when walking, running, bending, or kneeling.
What are the types of osteoarthritis?
There are actually two types of osteoarthritis (OA): primary and secondary.
Is osteoarthritis an inflammatory disease?
Osteoarthritis is an inflammatory disease. The inflammatory process found in OA has been studied for several decades. 1, 2 According to some recent studies,3, 4 OA behaves like an autoinflammatory disease, caused by responses mediated by chondrocytes and synoviocytes.
What is the most painful type of arthritis?
Rheumatoid arthritis can be one of the most painful types of arthritis; it affects joints as well as other surrounding tissues, including organs. This inflammatory, autoimmune disease attacks healthy cells by mistake, causing painful swelling in the joints, like hands, wrists and knees.
What are the 3 types of arthritis?
- Osteoarthritis. Osteoarthritis the most common form of arthritis. …
- Rheumatoid Arthritis. Rheumatoid arthritis is an autoimmune disease, which means that the immune system attacks parts of the body—especially the joints. …
- Psoriatic Arthritis.
What are 5 risk factors of arthritis?
- Family history. Some types of arthritis run in families, so you may be more likely to develop arthritis if your parents or siblings have the disorder.
- Age. …
- Your sex. …
- Previous joint injury. …
- Obesity.
Which form of arthritis is considered an autoimmune disease?
Rheumatoid arthritis is an autoimmune disease. Normally, your immune system helps protect your body from infection and disease. In rheumatoid arthritis, your immune system attacks healthy tissue in your joints. It can also cause medical problems with your heart, lungs, nerves, eyes and skin.
Do Rheumatologists treat osteoarthritis?
Rheumatologists – Rheumatologists specialize in musculoskeletal diseases and autoimmune conditions. They treat all types of arthritis, including osteoarthritis, rheumatoid arthritis and psoriatic arthritis. If there’s a chance you have something other than osteoarthritis, you will be sent to a rheumatologist.
Can osteoarthritis cause positive ANA?
When these tests return normal or negative results, this usually indicates that your arthritis is osteoarthritis. It should be noted, however, that as people age, they sometimes develop a low-level positive rheumatoid factor, ANA titer and/or elevated sedimentation rate without experiencing any obvious illness.
What causes early osteoarthritis?
The main causes of early-onset osteoarthritis include a history of joint trauma or injury, being overweight, and joint malalignment.



