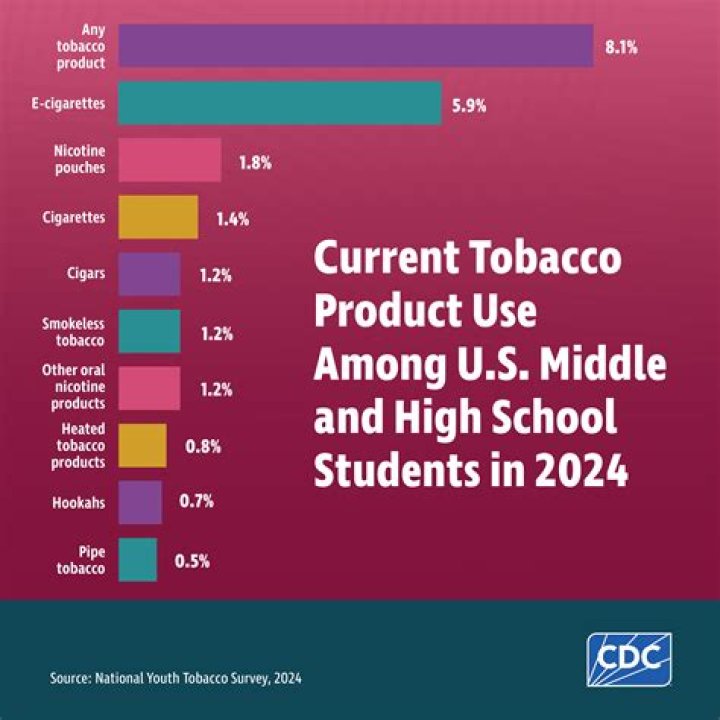
What nerves can be damaged in Lithotomy position
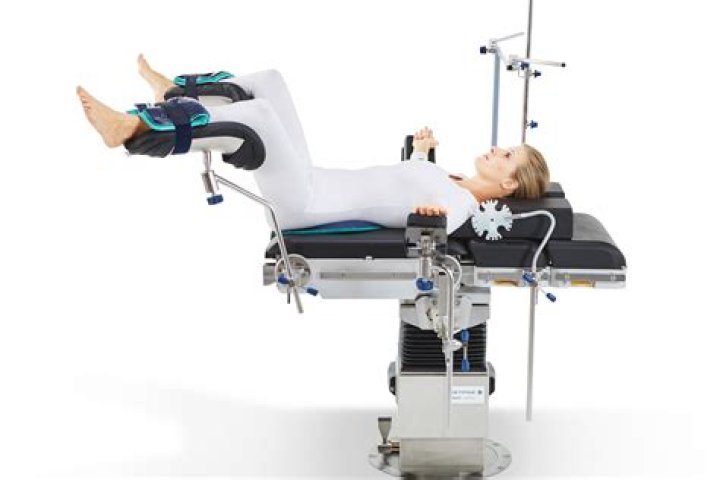
Neurologic injuries related to the lithotomy position may affect the femoral, sciatic, and common peroneal nerves. One series found that the most common lower extremity neuropathies associated with procedures in the lithotomy position were common peroneal (81%), sciatic (15%), and femoral (4%).
What are the anatomical risks in the lithotomy position?
The potential hazards to the patient in the lithotomy position are: skin breakdown, nerve damage, musculoskeletal injury (improper raising and lowering of the legs), and circulatory compromise. The patient may also experience hypotension if the legs are raised or lowered too quickly. Lateral position.
What is peroneal nerve damage?
A peroneal nerve injury is damage to the nerve on the outer part of the lower knee. This nerve sends impulses to and from the leg, foot, and toes. Damage can cause weakness, numbness, and pain. It may also make it hard for a person to lift their foot.
What nerves can be damaged in supine position?
Historically, the ulnar nerve was the most common nerve injured in the perioperative setting, followed by the brachial plexus and lumbosacral roots. Symptoms of ulnar neuropathy include paresthesia and weakness of the fourth and fifth digits of the affected hand, and pain of the medial forearm and hand.What is examined in lithotomy position?
The lithotomy position is a common position for surgical procedures and medical examinations involving the pelvis and lower abdomen, as well as a common position for childbirth in Western nations.
Which is a serious complication of being in the prone position?
Cardiovascular collapse, arrest. As mentioned above, prone position during surgery is associated with reduced stroke volume, cardiac index, raised central venous pressure and low blood pressure. This, when combined with other factors, is associated with an increased risk for cardiovascular collapse and arrest.
When positioning a patient for lithotomy care should be taken to avoid injury of the peroneal nerve which can cause injury to the?
(4) Compression of the common peroneal nerve is usually associated with the lithotomy position. Injury to the nerve can cause foot inversion and drop. Injury can be avoided by adequate padding of the stirrups and avoiding the lower legs resting against the stirrups.
What is a modified lithotomy position?
The modified lithotomy position frequently is used in general surgery because it gives excellent simultaneous access to the abdomen and perineum. There are a variety of complications that may occur including lumbosacral plexus stretch, sciatic and peroneal nerve injury, and compartment syndrome of the legs.What is the most common nerve injury for a patient in a lateral decubitus position?
Damage to brachial plexus is one of the most frequent positioning injuries when patients are in lateral decubitus position. Suprascapular neuropathy is easily overlooked injury. It occurs by circumduction of the arm across the chest or lateralization of the neck toward opposite shoulder.
Which nerve is most frequently injured as a result of improper positioning of the patients arms?The brachial plexus is the second most common pe- ripheral nerve to be injured due to improper positioning of the patient during general anesthesia, after the ul- nar nerve (1).
Article first time published onHow do you test for peroneal nerve damage?
To test for the motor involvement of the superficial peroneal nerve and deep peroneal nerve, one must assess foot eversion (SPN) and foot/toe dorsiflexion (DPN). A finding of weakness of both foot eversion as well as foot/toe dorsiflexion suggests a lesion involving the common peroneal nerve.
What are the symptoms of nerve damage in the knee?
Sensation changes in the thigh, knee, or leg, such as decreased sensation, numbness, tingling, burning, or pain. Weakness of the knee or leg, including difficulty going up and down stairs — especially down, with a feeling of the knee giving way or buckling.
What are the possible complications associated with the injury to common peroneal nerve?
Injuries to the peroneal nerve can cause numbness, tingling, pain, weakness and a gait problem called foot drop.
What is the primary purpose of slowly lowering a patient's legs from the lithotomy position?
The risk of nerve injury increases with every hour spent in the lithotomy position. Intraoperative position changes of the legs can minimize the time spent in lithotomy and potentially limit nerve injuries.
What is exaggerated lithotomy?
The exaggerated lithotomy position is used during radical perineal prostatectomy to increase perineal exposure. The aim of this study was to evaluate the effects of the exaggerated lithotomy position on respiratory mechanics and arterial blood gases.
Why would you put a patient in Trendelenburg position?
Positioning a patient for a surgical procedure involves reducing risk of injury and increasing comfort. The Trendelenburg position allows a surgeon greater access to pelvic organs, helpful for procedures like colorectal, gynecological, and genitourinary surgery.
Who is responsible for patient positioning during surgery?
Positioning the patient for a surgical procedure is a shared responsibility among the surgeon, the anesthesiologist, and the nurses in the operating room. The optimal position may require a compromise between the best position for surgical access and the position the patient can tolerate.
Why does Proning work for Covid?
Research has found that when proning is used in patients with severe ARDS and hypoxemia not improved by other means, it has the benefit of: better ventilation of the dorsal lung regions threatened by alveolar collapse; improvement in ventilation/perfusion matching; and. potentially an improvement in mortality.
What is a Lithotomy procedure?
The lithotomy position is often used during childbirth and surgery in the pelvic area. It involves lying on your back with your legs flexed 90 degrees at your hips. Your knees will be bent at 70 to 90 degrees, and padded foot rests attached to the table will support your legs.
What is a Jackson table?
The Jackson Table (Fig. 1) method encompasses sliding the patient from a cart onto the table with appropriate padding placed while the patient is strapped securely on the table. The carbon fiber table frame is placed over the patient, and the patient-table construct is sandwiched together.
What physiological effect is most likely to result from positioning a patient in Lithotomy position?
Lithotomy Position Hemodynamic changes include the increased venous return and transient increases in preload and cardiac output. Respiratory changes result from cephalad displacement of abdominal contents resulting in decreased lung compliance, functional residual capacity, and tidal volume.
What is perioperative positioning injury?
Potential for damage to skin, soft tissue, joints, ligaments, bones, eyes, nerves and blood and lymph vessels as a result of the mechanism of compression or stretching that occurs while positioning the patient to expose the surgical site especially in patients identified at risk for perioperative pressure injury. [
What should be checked routinely for patients in a lateral decubitus position?
The dependent eye should be routinely checked throughout the procedure to assess for any external compression. A detailed discussion of perioperative visual loss can be found in the section on prone positioning.
What Is Reverse Trendelenburg?
The Reverse Trendelenburg position is a position in which patients’ hip and knee are not flexed but the head and chest are elevated at 30° than the abdomen and legs.
What is dorsal Lithotomy?
When in the dorsal lithotomy position, a woman is putting direct pressure on her sacrum (tailbone), forcing it into a flexed position and making the pelvic outlet smaller.
What is Fowler's and supine?
Fowler’s position is commonly used for shoulder arthroscopy procedures. Surgical tables may be articulated to place patients in a seated position or shoulder chair (beach chair) accessories may be used as an alternative. The patient is placed supine on the operating table and general endotracheal anesthesia is induced.
Which nerve is most likely to be injured in the anesthetized patient who is in the sitting position?
Injury to the ulnar nerve may be the most common nerve injury associated with general anesthesia and a significant source of litigation. These injuries appear to occur in the absence of obvious trauma to the involved extremity and are often delayed in their clinical presentation.
What potential complication can occur while a patient is in a sitting position?
The classic sitting position causes postural hypotension in about 1/3 of patients, and 2–5% of patients suffer severe hypotension (decrease in blood pressure more than by half from baseline). (29) The major hemodynamic consequence is decrease in venous return, leading to decrease in cardiac output and hypotension.
Why is supine position important?
The supine position is one of the most natural positions for patients and usually allows for all patient anatomical structures to remain in natural neutral alignment. Most patients are able to maintain adequate respiratory function with no constricting external compression on the respiratory system.
Can peroneal nerve damage heal on its own?
Aim: Common peroneal nerve (CPN) injuries represent the most common nerve lesions of the lower limb and can be due to several causative mechanisms. Although in most cases they recover spontaneously, an irreversible damage of the nerve is also likely to occur.
How long does it take the peroneal nerve to heal?
The recovery time after a common peroneal nerve decompression at the knee is usually 3-4 months. For the first 6 weeks, we do not want to encourage the knee to form a lot of scar tissue around the area of the decompression, so we have patients on crutches.