What is weaning from mechanical ventilation
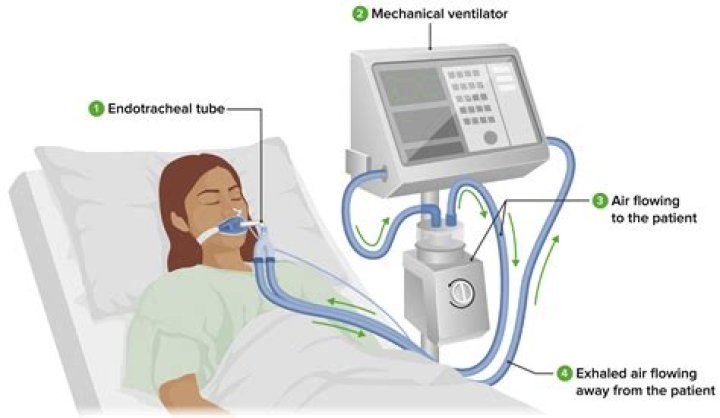
Weaning — Weaning is the process of decreasing the degree of ventilator support and allowing the patient to assume a greater proportion of their own ventilation (eg, spontaneous breathing trials or a gradual reduction in ventilator support).
What is the weaning process of mechanical ventilation?
Weaning from mechanical ventilation is the process of reducing ventilatory support, ultimately resulting in a patient breathing spontaneously and being extubated. This process can be achieved rapidly in ∼80% of patients when the original cause of the respiratory failure has improved.
How long does weaning off a ventilator take?
Weaning Success Average time to ventilator liberation varies with the severity and type of illness or injury, but typically ranges from 16 to 37 days after intubation for respiratory failure. If the patient fails to wean from ventilator dependence within 60 days, they will probably not do so later.
What does weaning off a ventilator mean?
Weaning from mechanical ventilation can be defined as the process of abruptly or gradually withdrawing ventilatory support.What is weaning protocol?
Weaning per protocol was defined as a method of limiting the duration of invasive ventilation that included at least the first two of: a list of objective criteria based on general clinical factors for deciding if a patient is ready to discontinue mechanical ventilation; structured guidelines for reducing ventilatory …
What is an indicator of weaning failure?
Weaning-failure patients are frequently unable to increase minute ventilation in response to high arterial partial pressure of carbon dioxide (PaCO2) because of respiratory muscle weakness, altered respiratory mechanics, and so on.
When weaning a patient what ventilator setting is commonly used?
Weaning techniques include spontaneous breathing trials (SBTs), pressure-support ventilation (PSV), and synchronized intermittent mandatory ventilation (SIMV).
What's your primary nursing responsibility when the patient is being weaned off from a mechanical ventilator?
Therefore, patients weaning from mechanical ventilators should be attached to a cardiac monitor to observe for arrhythmias and blood pressure changes. Fluid balance must also be maintained since adequate hydration is essential in effective recovery from critical illness and in secretion management.Can you be weaned off a ventilator?
How does someone come off a ventilator? A patient can be weaned off a ventilator when they’ve recovered enough to resume breathing on their own. Weaning begins gradually, meaning they stay connected to the ventilator but are given the opportunity to try to breathe on their own.
What are the weaning parameters?The most common weaning parameters to consider initiating the SBT are RSBI of less than 105, maximal inspiratory pressure (MIP) less than -30 cm of water, and minute ventilation less than 10 liters per minute.
Article first time published onWhat should be monitored when a patient is about to be weaned off a ventilator?
Parameters commonly used to assess a patient’s readiness to be weaned from mechanical ventilatory support include the following: Respiratory rate less than 25 breaths per minute. Tidal volume greater than 5 mL/kg. Vital capacity greater than 10 mL/k.
What happens after a ventilator is taken off?
People tend to stop breathing and die soon after a ventilator shuts off, though some do start breathing again on their own. If they are not taking in any fluids, they will usually die within several days of a feeding tube removal, though they may survive for as long as a week or two.
What is the purpose of a weaning trial?
Weaning — Weaning is the process of decreasing the degree of ventilator support and allowing the patient to assume a greater proportion of their own ventilation (eg, spontaneous breathing trials or a gradual reduction in ventilator support).
What sedation do you wean first?
Minimum sedation is the prerequisite for weaning and should be regarded in any case as the default target in the absence of special circumstances such as severe ARDS, TBI or use of NMBs. Use of longer-acting sedatives should be avoided.
What are the weaning modes?
Thus, the work of breathing is shifted from the ventilator to the patient. The three general approaches to weaning are the spontaneous breathing trial (SBT), pressure-support ventilation (PSV), and synchronized intermittent mandatory ventilation (SIMV).
When should you Extubate a patient?
Extubation should not be performed until it has been determined that the patient’s medical condition is stable, a weaning trial has been successful, the airway is patent, and any potential difficulties in reintubation have been identified.
What happens if a patient Cannot be weaned off a ventilator?
Failed weaning can be associated with the development of respiratory muscle fatigue, which could predispose to structural muscle injury and hinder future weaning efforts. In fact, it appears that fatigue rarely occurs during a well-monitored SBT as long as the patient is expeditiously returned to ventilatory support.
What is prolonged weaning?
Prolonged weaning, which includes patients who fail 3 SBTs or are still on mechanical ventilation 7 days after the first SBT, affects a relatively small fraction of mechanically ventilated ICU patients but these, however, requires disproportionate resources.
What is extubation failure?
Extubation failure is defined as inability to sustain spontaneous breathing after removal of the artificial airway; an endotracheal tube or tracheostomy tube; and need for reintubation within a specified time period: either within 24-72 h[1,2] or up to 7 days.
What is Extubation procedure?
Extubation is when the doctor takes out a tube that helps you breathe. Sometimes, because of illness, injury, or surgery, you need help to breathe. Your doctor or anesthesiologist (a doctor who puts you to “sleep” for surgery) puts a tube (endotracheal tube, or ETT) down your throat and into your windpipe.
How long can you live after being taken off a ventilator?
Time to death after withdrawal of mechanical ventilation varies widely, yet the majority of patients die within 24 hours. Subsequent validation of these predictors may help to inform family counseling at the end of life.
Can someone on a ventilator hear you?
They do hear you, so speak clearly and lovingly to your loved one. Patients from Critical Care Units frequently report clearly remembering hearing loved one’s talking to them during their hospitalization in the Critical Care Unit while on “life support” or ventilators.
What is the final stage of dying?
Active dying is the final phase of the dying process. While the pre-active stage lasts for about three weeks, the active stage of dying lasts roughly three days. By definition, actively dying patients are very close to death, and exhibit many signs and symptoms of near-death.
How do you wean yourself from sedation?
Weaning protocols for both sedation and ventilator weaning should be implemented in daily routine. The essential element of such algorithm should be a daily spontaneous awakening trial and spontaneous breathing trial. Furthermore, regularly monitoring for deepness of sedation and delirium should be implemented.



