What is the role of platelets in inflammation
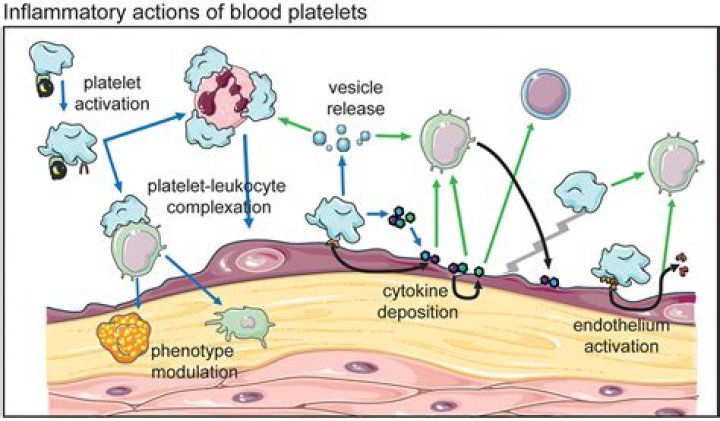
Platelets are important players in the development of inflammation. They store multiple inflammatory molecules that, upon release, chemoattract key innate immune cells leukocytes and stimulate endothelium. Platelets interact with leukocytes and support their interaction with vessel wall and egression to tissues.
Why are platelets high in inflammation?
Inflammatory Conditions 5 The elevated platelet count occurs in response to cytokines (small proteins released from cells that signal other cells to do something). In particular, the cytokines interleukin-6 and thrombopoietin stimulate platelet production.
Are platelets an inflammatory marker?
Platelets are considered an important source of prothrombotic agents associated with inflammatory markers, and play a role in the initiation and propagation of vascular and inflammatory diseases 5.
What is the major role of platelets?
Platelets play a major role in blood clotting. Normally, when one of your blood vessels is injured, you start to bleed. Your platelets will clot (clump together) to plug the hole in the blood vessel and stop the bleeding.Can inflammation lower platelets?
Aside from platelet numbers and its consequences on THPO levels, platelet activity is also affected throughout the course of inflammation. Although spontaneous platelet activity could be observed in severely septic patients, stimulus-dependent ex vivo aggregation of these platelets was significantly reduced (75).
What are the 3 functions of platelets?
While the primary function of the platelet is thought to be hemostasis, thrombosis, and wound healing through a complex activation process leading to integrin activation and formation of a “core” and “shell” at the site of injury, other physiological roles for the platelet exist including immunity and communication …
What is the role of platelets in immunity?
Platelets are known to influence the innate immune response through regulation of both the maturation and activation of such innate immune cells as macrophages, neutrophils, and dendritic cells [79, 86, 87].
What stimulates platelet production?
Thrombopoietin is a glycoprotein hormone produced by the liver and kidney which regulates the production of platelets. It stimulates the production and differentiation of megakaryocytes, the bone marrow cells that bud off large numbers of platelets.What is the function of erythrocyte?
Red blood cells, also known as erythrocytes, deliver oxygen to the tissues in your body. Oxygen turns into energy and your tissues release carbon dioxide. Your red blood cells also transport carbon dioxide to your lungs for you to exhale.
What is the principle inflammatory mediator released by platelets?Thromboxane and Prostaglandins COX is expressed in many inflammatory cells, but platelets are a major source of COX products in the vasculature. Platelets constitutively express COX-1 and during times of prolonged inflammation can express COX-2 (16).
Article first time published onWhat is called inflammation?
What Is Inflammation? Inflammation is a process by which your body’s white blood cells and the things they make protect you from infection from outside invaders, such as bacteria and viruses.
What are inflammatory markers?
Inflammatory markers include C reactive protein (CRP), erythrocyte sedimentation rate, plasma viscosity, fibrinogen, ferritin, and several other acute phase proteins, though only the first three are commonly referred to as inflammatory markers.
How do platelets protect the body from infection and disease?
Platelets sense invading pathogens through their receptors, which results in platelet activation. Activated platelets release antimicrobial proteins and molecules that regulate the host response against infection. Antimicrobial proteins directly target the pathogen to limit the spread of the infection.
Do platelets fight infection?
Platelets can bind and internalize pathogens and release microbicidal proteins that kill certain bacteria and fungi.
Does platelet count decrease in bacterial infection?
1,2 Infections cause decrease in platelet count both due to effects on platelet production and platelet survival. 3 Thrombocytopenia in bacterial infections can occur as a part of sepsis with disseminated intravascular coagulation.
Why are platelets called platelets?
Platelets are small, clear, irregularly-shaped cell fragments produced by larger precursor cells called megakaryocytes. Platelets are also called thrombocytes because they are involved in the blood clotting process, which is necessary for wound healing.
Are platelets red blood cells?
Unlike red and white blood cells, platelets are not actually cells but rather small fragments of cells. Platelets help the blood clotting process (or coagulation) by gathering at the site of an injury, sticking to the lining of the injured blood vessel, and forming a platform on which blood coagulation can occur.
What are the functions of RBC WBC and platelets?
Red blood cells are responsible for carrying oxygen and carbon dioxide. Platelets are responsible for blood clotting. White blood cells are part of the immune system and function in immune response.
Why RBC is called erythrocyte?
The term Erythrocytes (from the Gk erythros=red and kytos=cell) is used for RBCs because of their characteristic red colour which also gave blood its colour due to their abundance. … They are responsible for facilitating clotting of blood in case of wounds or seepage to prevent blood loss.
What is erythrocyte and leukocyte?
Red blood cells (erythrocytes). These carry oxygen from the lungs to the rest of the body. White blood cells (leukocytes). These help fight infections and aid in the immune process.
Which organ makes platelets?
Platelets are produced in your bone marrow. Factors that can decrease platelet production include: Leukemia and other cancers.
Why do steroids increase platelet count?
Corticosteroids (“steroids”) — Steroids prevent bleeding by decreasing the production of antibodies against platelets. If effective, the platelet count will rise within two to four weeks of starting steroids.
What medications affect platelet activation?
Drugs. Aspirin, other NSAIDs, inhibitors of the platelet P2Y12 adenosine diphosphate (ADP) receptor (eg, clopidogrel, prasugrel, ticagrelor), and glycoprotein IIb/IIIa receptor inhibitors (eg, abciximab, eptifibatide, tirofiban) may induce platelet dysfunction.
What happens during inflammatory response?
The inflammatory response (inflammation) occurs when tissues are injured by bacteria, trauma, toxins, heat, or any other cause. The damaged cells release chemicals including histamine, bradykinin, and prostaglandins. These chemicals cause blood vessels to leak fluid into the tissues, causing swelling.
What stimulates the inflammatory response?
The factors that can stimulate inflammation include microorganisms, physical agents, chemicals, inappropriate immunological responses, and tissue death. Infectious agents such as viruses and bacteria are some of the most common stimuli of inflammation.
What is the role of chemical mediators in inflammation?
In response to the inflammatory process, these cells release specialized substances which include vasoactive amines and peptides, eicosanoids, proinflammatory cytokines, and acute-phase proteins, which mediate the inflammatory process by preventing further tissue damage and ultimately resulting in healing and …
What is the purpose of inflammation?
Inflammation is the immune system’s response to harmful stimuli, such as pathogens, damaged cells, toxic compounds, or irradiation [1], and acts by removing injurious stimuli and initiating the healing process [2]. Inflammation is therefore a defense mechanism that is vital to health [3].
What are the 4 stages of inflammation?
The four cardinal signs of inflammation are swelling, pain, redness, and localized heat. Sometimes, loss of function is also evident.
What are the two types of inflammation?
There are two types of inflammation: acute and chronic. People are most familiar with acute inflammation. This is the redness, warmth, swelling, and pain around tissues and joints that occurs in response to an injury, like when you cut yourself.
What blood tests detect inflammation?
Erythrocyte sedimentation rate (ESR), C-reactive protein (CRP) and plasma viscosity (PV) blood tests are commonly used to detect increase in protein in the blood. In this way they are used as markers of inflammation.
Is ferritin an inflammatory marker?
Serum ferritin is an important inflammatory disease marker, as it is mainly a leakage product from damaged cells. Metallomics.



