What is the choriocarcinoma
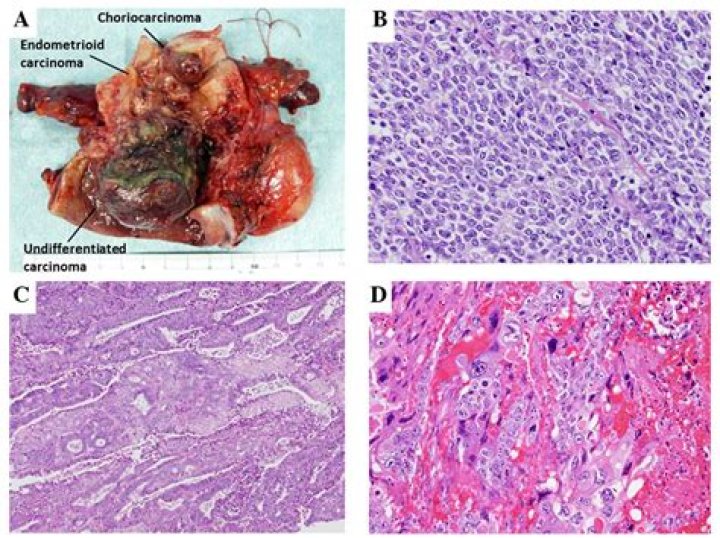
(KOR-ee-oh-KAR-sih-NOH-muh) A malignant, fast-growing tumor that develops from trophoblastic cells (cells that help an embryo attach to the uterus and help form the placenta). Almost all choriocarcinomas form in the uterus after fertilization of an egg by a sperm, but a small number form in a testis or an ovary.
What causes choriocarcinoma?
What Causes It? Choriocarcinoma forms when cells that were part of the placenta in a normal pregnancy become cancerous. It can happen after a miscarriage, abortion, ectopic pregnancy, or molar pregnancy — when an egg is fertilized, but the placenta develops into a mass of cysts instead of a fetus.
Is choriocarcinoma cancer curable?
Choriocarcinoma is a rare type of cancer. It usually develops from cells that remain inside the body after a pregnancy. In the vast majority of cases, choriocarcinoma is curable. The outlook for people with this condition is generally very good, although it can sometimes cause complications.
What happens in choriocarcinoma?
Choriocarcinoma is a fast-growing cancer that occurs in a woman’s uterus (womb). The abnormal cells start in the tissue that would normally become the placenta. This is the organ that develops during pregnancy to feed the fetus.Who is at risk of choriocarcinoma?
The risk of complete molar pregnancy is highest in women over age 35 and younger than 20. The risk is even higher for women over age 45. Age is less likely to be a factor for partial moles. For choriocarcinoma, risk is lower before age 25, and then increases with age until menopause.
How quickly does choriocarcinoma spread?
Choriocarcinoma can develop some months or even years after pregnancy and can be difficult to diagnose, because it is so unexpected. They can grow quickly and might cause symptoms within a short period of time. They can spread to other parts of the body but are very likely to be cured by chemotherapy treatment.
How long is the treatment for choriocarcinoma?
Treatment for choriocarcinoma usually takes 4-5 months to complete and the cure rate is over 95%.
Can Stage 4 choriocarcinoma be cured?
Fortunately, most women who are found to have choriocarcinoma can be cured; treatment with a combination of chemotherapy agents such as etoposide, methotrexate, actinomycin D, cyclophosphamide and vincristine (EMA-CO) is found to be very effective at achieving remission.Is choriocarcinoma serious?
Choriocarcinoma is a very rare type of cancer that occurs in around 1 in 50,000 pregnancies. It can develop if the cells left behind after a pregnancy become cancerous.
Is choriocarcinoma benign or malignant?Unlike a hydatidiform mole, a choriocarcinoma is a malignant and more aggressive form of GTD that spreads into the muscle wall of the uterus. A choriocarcinoma can also spread more widely to other parts of the body such as the lungs, liver, and/or brain.
Article first time published onIs choriocarcinoma hereditary?
The genetic contributions to the choriocarcinoma were determined by comparing the genotypes of the choriocarcinoma and that of the couples. Results: Four of twelve cases had only a maternal contribution, indicating a non-gestational origin.
What are the symptoms of choriocarcinoma?
- lungs – you might have a cough, difficulty breathing and sometimes chest pain.
- vagina – you might have heavy bleeding, and your doctor might be able to feel a lump (nodules) in your vagina.
- abdomen – you might have abdominal pain.
Is choriocarcinoma a germ cell tumor?
Overview. Choriocarcinoma of the testis is a germ cell tumor that is rarely identified in its pure form; it is more often seen as a component of a nonseminomatous germ cell tumor.
How do you manage choriocarcinoma?
- Combination chemotherapy.
- Intrathecal chemotherapy and radiation therapy to the brain (for cancer that has spread to the lung, to keep it from spreading to the brain).
Can choriocarcinoma be seen on ultrasound?
An ultrasound scan can diagnose many women with persistent trophoblastic disease or choriocarcinoma.
What are the chances of getting choriocarcinoma?
Choriocarcinomas are extremely rare and develop from cells of the placenta. They happen after 1 in 50,000 pregnancies.
What chemotherapy is used for choriocarcinoma?
If you have high risk PTD or choriocarcinoma, you might have the drug methotrexate by drip into a vein (intravenous infusion). This is followed a week later by the drugs actinomycin and etoposide. Or you may have a combination of chemotherapy drugs called EMA-CO.
How do doctors do chemotherapy?
Chemotherapy is most often given as an infusion into a vein (intravenously). The drugs can be given by inserting a tube with a needle into a vein in your arm or into a device in a vein in your chest. Chemotherapy pills. Some chemotherapy drugs can be taken in pill or capsule form.
Is methotrexate used in choriocarcinoma?
Conclusion: Methotrexate is routinely used in a parenteral intramuscular fashion for the treatment of gestational choriocarcinoma. Physicians should be aware that, in very limited situations, oral methotrexate in combination with hysterectomy still could offer a patient successful treatment for stage III GTN.
Are all cancers carcinomas?
Not all cancers are carcinoma. Other types of cancer that aren’t carcinomas invade the body in different ways. Those cancers begin in other types of tissue, such as: Bone.
Is a molar pregnancy a real baby?
Complete molar pregnancies have only placental parts (there is no baby) and form when the sperm fertilizes an empty egg. Because the egg is empty, no baby is formed. The placenta grows and produces the pregnancy hormone, hCG. Unfortunately, an ultrasound will show that there is no fetus, only a placenta.
Can males get choriocarcinoma?
Primary choriocarcinoma (PCC) is a rare malignancy that can occur in both men and women. In men, the most common primary site is the testis. When the primary tumor is extragonadal, it can occur in the mediastinum,2 retroperitoneum,3 lung,4 brain,5 or digestive tract.
Is GTD curable?
GTD is typically curable, especially when found early. The main treatments for GTD are surgery and/or chemotherapy. Descriptions of the common types of treatments used for GTD are listed below. Your care plan may include treatment for symptoms and side effects, an important part of medical care.
Where does rhabdomyosarcoma occur?
Rhabdomyosarcoma (RMS or “Rhabdo”) is a cancerous tumor that develops in the body’s soft tissues, usually the muscles. It can affect the head, neck, bladder, vagina, arms, legs, trunk, or just about any body part.
What is choriocarcinoma stage4?
Choriocarcinoma is the most malignant tumor of gestational trophoblastic disease arising from any gestation. It has a tendency toward relapse as well as metastasis. Here, a case of relapsed high-risk choriocarcinoma (FIGO stage IV, WHO score 12) in a 37-year-old female presenting with vaginal bleedings is described.
Is H mole safe?
Partial and complete hydatidiform moles are benign (not cancerous) forms of GTD. However, there is a risk that a hydatidiform mole can develop into a cancerous (malignant) type of GTD, known as gestational trophoblastic neoplasia (GTN).
What is an invasive mole?
Invasive mole is a subtype of gestational trophoblastic neoplasms (GTNs) that usually develops from the malignant transformation of trophoblastic tissue after molar evacuation. Invasive moles mostly occur in women of reproductive age, while they are extremely rare in postmenopausal women.
What is a trophoblast?
Listen to pronunciation. (TROH-foh-BLAST) A thin layer of cells that helps a developing embryo attach to the wall of the uterus, protects the embryo, and forms a part of the placenta.
How can you tell the difference between choriocarcinoma and invasive mole?
Invasive mole is unlike choriocarcinoma, the latter is without the presence of chorionic villi. It is important to distinguish between invasive mole and choriocarcinoma, as the former has a more favorable outcome.
Where can molar pregnancy spread?
This type of tumor grows slowly, but it can eventually spread to the uterine muscle, nearby blood vessels, and lymph nodes, pelvis, or lungs. Signs and symptoms may not occur until well after a normal pregnancy, an abortion, or treatment for a molar pregnancy.
What is trophoblastic proliferation?
Oncology. Gestational trophoblastic disease (GTD) is a term used for a group of pregnancy-related tumours. These tumours are rare, and they appear when cells in the womb start to proliferate uncontrollably.