What is the best treatment for pustular psoriasis
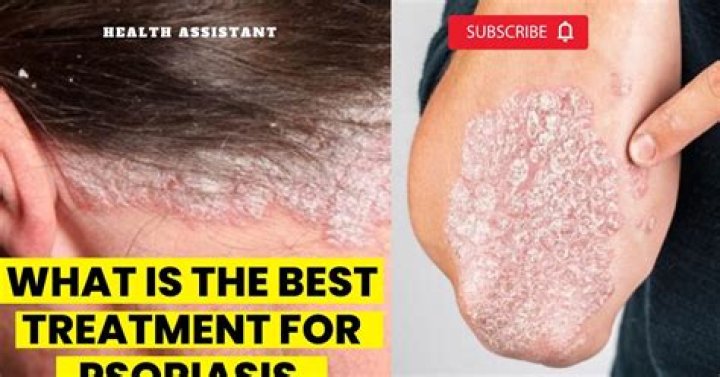
Pustular psoriasis usually needs medical treatment, but some home remedies may offer additional relief by soothing the skin and relieving irritation and itching. Possible options include: bathing with salt water. taking oatmeal baths.
How do you treat pustular psoriasis at home?
Pustular psoriasis usually needs medical treatment, but some home remedies may offer additional relief by soothing the skin and relieving irritation and itching. Possible options include: bathing with salt water. taking oatmeal baths.
Which biologic is best for pustular psoriasis?
Anti-TNF-α is the most available biologics for the treatment of pustular psoriasis, and anti-IL-12/23 and anti-IL-17A might be considered as the first- or second-line therapy for moderate-to-severe and refractory pustular psoriasis.
What is the fluid in pustular psoriasis?
A pustular psoriasis is an uncommon form of psoriasis. Pustular psoriasis appears as clearly defined, raised bumps that are filled with a white, thick fluid composed of white blood cells. This purulent exudate is commonly called pus. The skin under and around these bumps is red.Can you cure pustular psoriasis?
Topicals, phototherapy, oral treatments and biologics are all possible treatment options for pustular psoriasis. You and your health care provider will discuss the best treatment plan for you based on the severity of your symptoms and your medical history.
How do you treat pustular eczema?
When dyshidrotic eczema is severe or flares happen often, dermatologists may prescribe light therapy, topical calcineurin inhibitors (TCIs) or oral steroids. Occasionally, botulinum toxin injections are used to control the sweaty hands and feet that can trigger the condition.
How do you treat pustular psoriasis on feet?
- Corticosteroid (apply to the skin)
- Synthetic vitamin D (apply to the skin)
- Phototherapy (light treatments)
- Corticosteroid and salicylic acid (apply to the skin)
What medications can cause pustular psoriasis?
- Pain or fever reducers with aspirin.
- Nonsteroidal anti-inflammatory drugs (ibuprofen, naproxen)
- Some anti-depressants like lithium or trazodone)
- Penicillin (antibiotic)
- Calcipotriol (a psoriasis drug)
- Coal tar (also used to treat psoriasis)
When should I go to the hospital for pustular psoriasis?
Pustular Psoriasis: Emergency Symptoms Go to the hospital immediately if the bumps spread quickly all over your body. Other emergency symptoms are severe itching, rapid pulse, fever, muscle weakness, and chills.
How long do you stay on biologics for psoriasis?The authors concluded that a maintenance dosing of infliximab every 8 weeks would be appropriate to maintain a meaningful clinical response. Median Psoriasis Area and Severity Index (PASI) with infliximab treatment at weeks 0, 2, and 6.
Article first time published onCan Erythroderma be cured?
Erythrodermic psoriasis can be difficult to treat, especially if complications develop. Treatments include topical treatments and drug therapy. A person’s treatment options will depend on the severity of their symptoms and the presence of any other health conditions.
What is the safest drug for psoriasis?
Options including certolizumab pegol (Cimzia), etanercept (Enbrel), adalimumab (Humira), and infliximab (Remicade) have been shown to be safe and effective when taken with methotrexate.
How do you treat pustular rosacea?
For moderate papulopustular rosacea, combination therapy with oral tetracyclines and topical agents is the first-line choice. Treatment with a topical agent, such as metronidazole, may help maintain remission. Patients with ocular involvement may benefit from long-term oral antibiotics and metronidazole gel.
What causes severe pustular psoriasis?
Causes and Triggers A few things can trigger psoriasis flares: Medications, such as steroids. Something that irritates your skin, like a topical cream or harsh skin care product. Too much sunlight.
Why do I get pustules?
What causes pustules to form? Pustules may form when your skin becomes inflamed as a result of an allergic reaction to food, environmental allergens, or poisonous insect bites. However, the most common cause of pustules is acne. Acne develops when the pores of your skin become clogged with oil and dead skin cells.
Which ointment is best for psoriasis?
- MG217 Medicated Multi-Symptom Moisturizing Cream.
- Curél Hydra Therapy Wet Skin Moisturizer.
- CeraVe Psoriasis Moisturizing Cream.
- Psoriasin Deep Moisturizing Ointment.
- Wynzora.
- Bioderma Atoderm Cream.
- MG217 Psoriasis Coal Tar Medicated Ointment.
- Cetaphil Hydrating Eye Gel Cream.
What is the code for pustular generalized psoriasis?
2022 ICD-10-CM Diagnosis Code L40. 1: Generalized pustular psoriasis.
Do pustules go away?
Pustules are irritating but otherwise harmless, and they usually go away on their own. People can often prevent them or reduce their severity by keeping pustule-prone areas clean and oil free. Many OTC treatments contain ingredients that can be effective against pustules.
Is Vaseline good for eczema?
Petroleum jelly is well tolerated and works well for sensitive skin, which makes it an ideal treatment for eczema flare-ups. Unlike some products that can sting and cause discomfort, petroleum jelly has moisturizing and soothing properties that alleviate irritation, redness, and discomfort.
What organs can be affected by psoriasis?
Psoriasis is an autoimmune condition that causes widespread inflammation. This can affect the skin and several other parts of the body, including the lungs.
Does ibuprofen help with psoriasis?
Nonsteroidal anti-inflammatory drugs (NSAIDs) like Advil or Motrin (ibuprofen) and aspirin, can ease psoriatic arthritis pain, but they won’t improve psoriasis.
Can you take antibiotics for psoriasis?
You may need antibiotics to treat the infection, but you shouldn’t take them solely to clear up psoriasis. Antibiotics haven’t been proven to work on guttate psoriasis. You shouldn’t take antibiotics for a condition they don’t effectively treat.
Can you take melatonin if you have psoriasis?
Our results indicate that nighttime melatonin levels are significantly lowered in psoriasis. Hence, our findings suggest that there is a role for melatonin agonists such as agomelatine and agents which modulate melatonin secretion, as an adjunct to standard therapy in patients with psoriasis and its co-morbidities.
What is the safest biologic drug?
The biologics Enbrel, Humira and Remicade are shown to be safe and effective when taken with methotrexate. This means that their biosimilars, including Erelzi, Amjevita, and Inflectra, may be safe and effective when taken with methotrexate.
Do you have to take biologics forever?
They require a subcutaneous injection or intravenous infusion. You should continue taking your biologic even while in remission, unless instructed otherwise by your doctor.
Are Biologics safe long-term?
Lack of long-term data While studies and clinical information indicate that biologics are generally safe, they are relatively new drugs, so — with the exception of Remicade (infliximab) — long-term safety information is not available.
Is erythroderma life-threatening?
Erythroderma is a severe inflammation of most of the body’s skin surface. It causes redness and scaling of the skin. This starts in patches and spreads over the body. Erythroderma can be life-threatening.
What is acitretin?
Acitretin is an oral retinoid (vitamin-A derivative) used to treat severe psoriasis, usually at a dose of 0.25–1 mg per kg body weight per day. It is best taken after a meal because it needs fat to be absorbed through the gut wall. Acitretin is available as 10 mg and 25 mg capsules.
Can your legs swell from psoriasis?
Complications to watch out for. Erythrodermic psoriasis can disrupt your body’s fluid balance and temperature regulation. This could lead to complications like: swelling under the skin, especially in the lower legs and feet, from fluid buildup (edema)
How long do you have to take Cosentyx?
The recommended dose for plaque psoriasis is 300 mg (two 150-mg injections) every week for five weeks. After week 5, you’ll need two 150-mg injections of Cosentyx once every four weeks.
Are there injections for psoriasis?
If you have moderate to severe psoriasis that hasn’t cleared with topical treatments, your doctor might recommend an injectable drug. Injectable drugs such as methotrexate (Otrexup, Rasuvo, and Trexall) and biologics can help clear up plaques and reduce inflammation.