What is Perilimbal injection
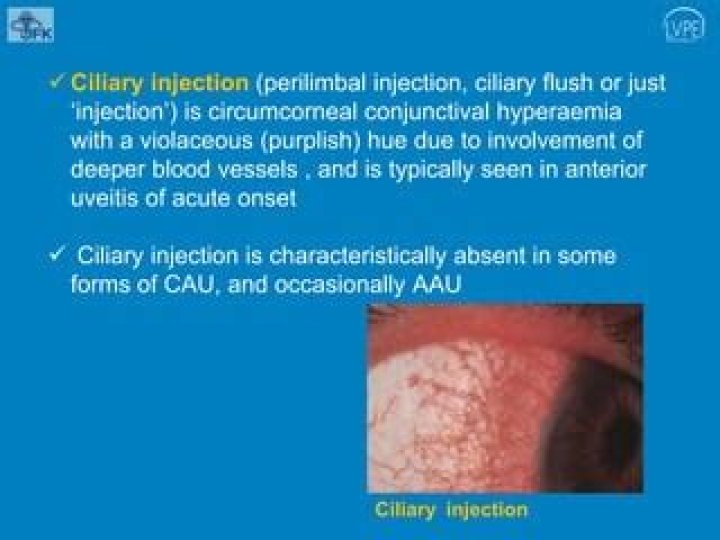
The eye exam will show conjunctival injection, worse around the limbus, which is the area of the conjunctiva adjacent to the iris. This is called perilimbal injection or ciliary flush.
What is Perilimbal flush?
One key finding that distinguishes uveitis from conjunctivitis, which is a far more common condition, is the presence of a perilimbal flush (an intense infection in the bulbar conjunctiva immediately adjacent to the cornea). A perilimbal flush may also occur with various forms of keratitis.
What causes uveitis?
Possible causes of uveitis are infection, injury, or an autoimmune or inflammatory disease. Many times a cause can’t be identified. Uveitis can be serious, leading to permanent vision loss. Early diagnosis and treatment are important to prevent complications and preserve your vision.
Can uveitis cause death?
No deaths due to iritis or uveitis have been reported. Morbidity results from posterior synechiae formation (adhesions between the iris and the lens) that may lead to high intraocular pressure and subsequent optic nerve loss. Blindness may result from inadequate treatment.What is the cause of Iridocyclitis?
Sometimes, it’s tied to eye trauma or other health conditions. Causes of iritis may include: Injury from burns, punctures, or strikes with a blunt object. Conditions such as ankylosing spondylitis, Reiter syndrome, sarcoidosis, inflammatory bowel disease, Behcet’s disease, juvenile rheumatoid arthritis, and psoriasis.
Where is the uveal tract located?
The uveal tract is the middle layer of the eye, divided into the anterior uvea (iris, ciliary body) and posterior uvea (choroid). The uvea is sandwiched between an outer layer (sclera) and an inner layer (retina).
Is iritis an autoimmune disease?
This autoimmune disease involves the growth of collections of inflammatory cells in areas of your body, including your eyes. Certain medications. Some drugs, such as the antibiotic rifabutin (Mycobutin) and the antiviral medication cidofovir, that are used to treat HIV infections can be a rare cause of iritis.
How long will uveitis last?
Uveitis symptoms may occur quickly in an acute form (lasts less than six weeks) or slowly in a chronic form (lasts longer than six weeks). These symptoms may get worse fast, and also may affect one or both eyes. The signs and symptoms of uveitis include: Eye redness.Is there a permanent cure for uveitis?
Treatment Strategies Even though there may not be a permanent cure for Uveitis, each attack can be treated, depending upon the cause, severity and location of the inflammation. The treatment may include eye drops, injections under the eye or oral medication.
How long does uveitis last with treatment?The part of your eye affected by uveitis will determine the duration of the condition. With proper treatment, anterior uveitis can clear up in a matter of days to weeks. Posterior uveitis, on the other hand, may last several months or years and could permanently alter your vision.
Article first time published onHow long does it take to go blind from uveitis?
The mean duration of visual loss was 20.35 months for patients with moderate visual loss and 22.8 months in patients with severe loss of vision. In patients with unilateral visual loss the mean duration was 20 months whereas it was 42.61 months in patients with bilateral visual morbidity.
What blood tests are done for uveitis?
- Blood count, overall biochemistry and erythrocyte sedimentation rate (ESR). …
- Antinuclear antibodies (ANA), antineutrophil cytoplasmic antibodies (ANCAs), antiphospholipid antibodies. …
- ACE and lysozyme. …
- Histocompatibility antigens. …
- Specific serological tests. …
- Skin tests.
What does uveitis pain feel like?
One of the signs of uveitis is eye pain. This is typically a sharp pain. Uveitis pain may come on suddenly, or it may be slow in onset with little pain, but gradual blurring of vision.
What is primary Iridocyclitis?
DEFINITION. Primary iridocyclitis is also know as uveitis. It represents an inflammation of the uveal tissues, primarily the iris and the ciliary body and is associated with the following conditions: Underlying systemic disease. Autoimmunity.
Is Iridocyclitis serious?
Iritis is the most common type of uveitis and generally occurs in healthy people. It can affect one eye, or it may affect both eyes at once. Iritis is usually the least serious type of uveitis.
Is Iridocyclitis a disease?
Iridocyclitis occurs when both the iris and ciliary body become inflamed. This can happen due to an injury, infection, a related condition such as arthritis, or for no apparent reason. Iridocyclitis can make eyes red, painful, and sensitive to light. And in rare cases, it can eventually lead to vision loss.
How do you prevent iritis?
Can iritis be prevented? There is not much you can do to prevent iritis. If you have an autoimmune condition, taking your medicines as prescribed may help prevent iritis. You may reduce your chance for problems if you see your eye care provider at the first sign of symptoms.
Can iritis make you tired?
Common symptoms include fatigue, weight loss, fever, chest pain, and difficulty breathing. It may also affect the skin, joints, and abdomen. Uveitis may involve any portion of the eye and it may lead to blurred vision, red eye, light sensitivity, pain, and floaters.
Can a damaged iris be repaired?
Iris surgeries come in the form of iris repair (iridoplasty) or an iris prosthesis. Iris repair often involves the use of sutures inside the eye to reshape the iris to its original shape, re-creating a round pupil. Sometimes the surgeon may cut some of the existing iris to help improve the appearance.
What is the function of uveal tract?
It is the source of blood flow to the ocular tissues. It is the source of aqueous humour (fluid that fills the inside of the eye) and maintenance of intraocular pressure. It constitutes the blood-aqueous barrier and prevents undesired blood products from reaching the eye.
What does the uveal tract do?
Function. The prime functions of the uveal tract as a unit are: Nutrition and gas exchange: uveal vessels directly perfuse the ciliary body and iris, to support their metabolic needs, and indirectly supply diffusible nutrients to the outer retina, sclera, and lens, which lack any intrinsic blood supply.
Why is it called uveal tract?
The uveal tract, or simply uvea, is the pigmented middle membrane of the layers that make up the eye. The uveal tract is also called the vascular tunic of the eye because it is rich in its blood supply – i.e., vascular – and because it envelops the eye like a tunic would cover a body.
What antibiotics treat uveitis?
DrugTarget site; mechanism of actionTime for re-treatment if needed (hours)AntibacterialsVancomycin2, 120Cell wall; prevents polymerization of peptidoglycan36-72Ceftazidime134Cell wall; inhibits the transpeptidase reaction48-72Amikacin103,129Protein synthesis; binds to the 30s ribosomal subunit of bacteria36-60
What is the home remedy for eye inflammation?
- Salt water. Salt water, or saline, is one of the most effective home remedies for eye infections. …
- Tea bags. …
- Warm compress. …
- Cold compress. …
- Wash linens. …
- Discard makeup.
What medications can cause uveitis?
These medications include cidofovir, cobalt, diethylcarbamazepine, pamidronic acid (disodium pamidronate), interleukin-3 and interleukin-6, oral contraceptives, quinidine, rifabutin, streptokinase and sulfonamides. Other systemic medications may cause uveitis.
Does uveitis require surgery?
Surgery. Rarely, an operation called a vitrectomy may be needed to treat uveitis. It’s usually only recommended if you have repeated or severe uveitis, or if the condition is caused by certain infections.
How do I get rid of uveitis?
- Antibiotics, antivirals or antifungals: These medications treat uveitis caused by an infection.
- Eye drops: Dilating (widening) the pupils with eye drops can reduce pain and swelling. …
- Steroidal anti-inflammatories: Medications that contain corticosteroids (steroids) alleviate eye inflammation.
Can I drive with uveitis?
Most patients with uveitis are able to continue driving. However, you have a duty to inform the DVLA if your vision drops below the legal limit of driving due to uveitis.
Can optometrists treat uveitis?
However, from the perspective of full scope optometry, providing the best care for your patient, and educating the patient that you can treat myriad diseases, the management of uveitis can be a practice builder in and of itself.
How is uveitis diagnosed?
- an eye chart or visual acuity test,
- a funduscopic exam,
- ocular pressure test,
- a slit lamp exam.
Can uveitis cause headaches?
However, in cases of chronic indolent uveitis the eye may be white and there may be minimal symptoms. The pain is mostly a constant, dull, aching pain that is moderate to severe and that some patients refer to as a headache. A few patients may complain of floaters in front of the eyes.