What is KT V in peritoneal dialysis
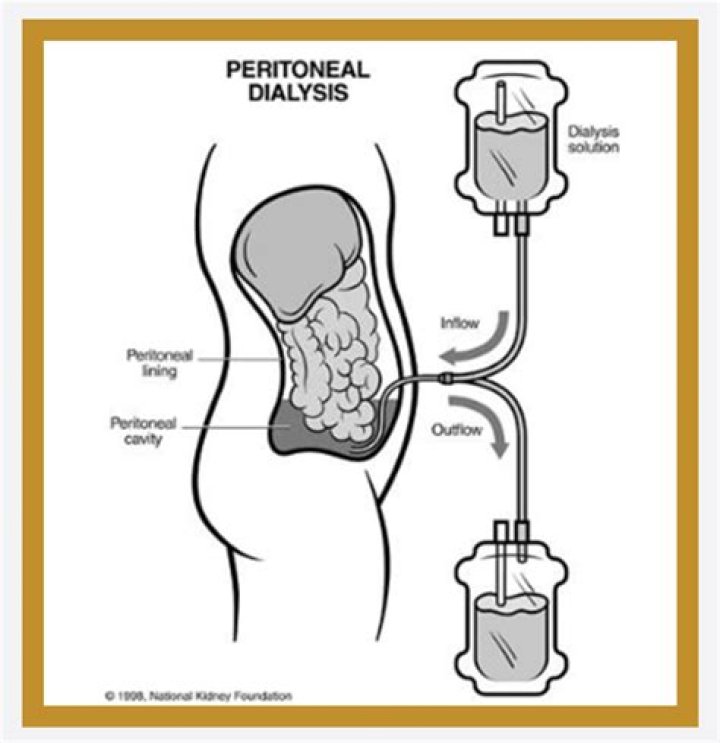
One way to assess adequacy of dialysis is to do a test called the Peritoneal Dialysis Adequacy Test. It is also called Kt/V. This test measures the waste products in your urine and dialysis drainage. It also measures protein nutrition and is able to assess how well you are eating.
What does KTV mean in dialysis?
Kt/V is another way of measuring dialysis adequacy. In this measurement, K stands for the dialyzer clearance, the rate at which blood passes through the dialyzer, expressed in milliliters per minute (mL/min)
How do you increase adequacy in peritoneal dialysis?
As with hemodialysis, patient size will influence the dose of dialysis needed to meet adequacy targets. In PD, we can increase the dose of dialysis by increasing the liters of dialysis used per day– either by increasing the fill volume or performing more exchanges per day.
What is Target kt V?
In hemodialysis the US National Kidney Foundation Kt/V target is ≥ 1.3, so that one can be sure that the delivered dose is at least 1.2. In peritoneal dialysis the target is ≥ 1.7/week.What is equilibrated Kt V?
Equilibrated Kt/V (eKt/V) The difference between the blood urea concentration at the end of dialysis and the concentration after full equilibration is referred to as “urea rebound”.
How do you calculate KT V in peritoneal dialysis?
(Renal Kt/V urea + dialysate Kt/V urea = total Kt/V urea for each patient.) This sum gives the total dialysis ‘adequacy’, as measured by urea clearance. Although this is not necessarily an ideal measurement of adequacy, it is the current measurement from which regulatory bodies assess peritoneal dialysis clearances.
How do you calculate KT over V?
The Kt/V can be resolved from the predialysis to postdialysis urea nitrogen ratio (R), the weight loss (UF), session length in hours (t), and anthropometric or modeled volume (V) using the equation: KtV = In (R – 0.008 x t) + (4 – 3.5 x R) x 0.55 UF/V.
What is the highest creatinine level before dialysis?
Creatinine levels that reach 2.0 or more in babies and 5.0 or more in adults may indicate severe kidney impairment. The need for a dialysis machine to remove wastes from the blood is based upon several considerations including the BUN, creatinine level, the potassium level and how much fluid the patient is retaining.What is double pool Kt V?
Double-pool kinetic modelling, represented by the concept of equilibrated Kt/V (eKt/V), addresses urea rebound by incorporating an equilibrated BUN (eqBUN) value drawn at 60 min post-dialysis, when urea rebound is nearly complete, making eKt/V a more accurate reflection of the ‘true’ urea mass removed by haemodialysis …
How do you know if your body is rejecting dialysis?In kidney failure some of you may have nausea, vomiting, a loss of appetite, weakness, increasing tiredness, itching, muscle cramps (especially in the legs) and anemia (a low blood count). With treatment for kidney failure, these symptoms will improve and you will begin to feel much better.
Article first time published onWhat is last fill volume in peritoneal dialysis?
Traditionally, peritoneal dialysis is performed using a volume of 2 l of fluid, containing glucose as an osmotic agent and lactate as a buffer.
Can you skip a day of peritoneal dialysis?
They either skip exchanges or sometimes skip entire treatment days when using CCPD. Skipping PD treatments has been shown to increase the risk of hospitalization and death.
What is Tenckhoff catheter?
The Tenckhoff catheter is a long, narrow tube inserted into you peritoneal cavity. The peritoneal cavity is the space in your body that contains your stomach, bowel, liver, bladder etc. It is covered by a membrane that holds all the organs in place—the peritoneal membrane.
What is eKdrt V?
eKdrt/V = dialysis and renal contribution both to eKt/V. stdKt/V = Standard Kt/V= the continuous clearance which is therapeutically equivalent to any schedule (number of dialyses per week) and intensity (eKt/V per dialysis) of intermittent dialysis therapy.
What affects KT V?
In addition to proper sampling tech- niques, BFR, time of treatment, volume of fluid removed, and a patient’s weight all affect the measurement of Kt/V.
How often is PD adequacy checked?
An adequacy test is done about 1 month after you finish your peritoneal dialysis training. It is also done every 6 months after that. Each time there is a change in your dialysis prescription your doctor may request your test be repeated.
What level of urea indicates kidney failure?
A GFR below 60 is a sign that the kidneys are not working properly. Once the GFR decreases below 15, one is at high risk for needing treatment for kidney failure, such as dialysis or a kidney transplant. Urea nitrogen comes from the breakdown of protein in the foods you eat. A normal BUN level is between 7 and 20.
What is UF volume in dialysis?
The UF volume is the amount of water that must be removed in a single treatment to return a patient to his or her target (or base) weight. The ultrafiltration volume is commonly expressed in terms of weight (where 1 litre = 1 kilogram). The UF rate is the speed at which that volume is removed.
How much blood do you lose during dialysis?
In hemodialysis, blood is removed from the body and filtered through a man-made membrane called a dialyzer, or artificial kidney, and then the filtered blood is returned to the body. The average person has about 10 to 12 pints of blood; during dialysis only one pint (about two cups) is outside of the body at a time.
What is PD adequacy?
Background: The current standard of adequacy for peritoneal dialysis (PD) is to provide a weekly normalized urea clearance (Kt/V) of 2.0 or more and a creatinine clearance (CCr) of 60 liter/1.73 m2 or more.
How do you calculate single pool Kt V?
Standard Kt/V is defined as the modeled urea nitrogen generation rate (g) in mg/min divided by the average pre-dialysis BUN, multiplied by 10 080 and divided by V [5].
What treatment factors decrease K?
- Absolute aldosterone deficiency or resistance to aldosterone effects.
- Low sodium delivery to the collecting duct.
- Low urine flow.
- Low serum potassium levels.
- Renal failure.
Is 300 creatinine level high?
Less that 30 mg is normal. 30–300 mg may mean early CKD. More than 300 mg may mean a later stage of CKD. Albumin to Creatinine Ratio.
What is normal creatinine after dialysis?
The mean creatinine and BUN levels after cessation of dialysis were 2.85 ± 0.57 mg/dl and 29.62 ± 5.26 mg/dl, respectively, while the mean creatinine clearance calculated by 24-hour urine collection was 29.75 ± 4.78 ml/min.
Is 2.2 creatinine level bad?
Creatinine Normal Range The normal levels of creatinine in the blood are 0.6 to 1.2 milligrams (mg) per deciliter (dL) in adult males and 0.5 to 1.1 mg/dL in adult females.
Can kidneys start working again after dialysis?
The good news is that acute kidney failure can often be reversed. The kidneys usually start working again within several weeks to months after the underlying cause has been treated. Dialysis is needed until then.
What is the most common cause of death in dialysis patients?
Cardiovascular disease is the leading cause of death in dialysis patients and sudden death (SD) represents a significant proportion of overall mortality in both hemodialysis (HD) and peritoneal dialysis (PD) patients.
Does dialysis remove creatinine?
Dialysis removes fluid and wastes Waste such as nitrogen and creatinine build up in the bloodstream. If you have been diagnosed with CKD, your doctor will have these levels carefully monitored. One of the best indicators of kidney function is your glomerular filtration rate (GFR).
How much fluid is removed during peritoneal dialysis?
You do the treatment by placing about two quarts of cleansing fluid into your belly and later draining it. This is done by hooking up a plastic bag of cleansing fluid to the tube in your belly.
Why is my PD catheter not draining?
Outflow failure is attributed mostly to mechanical problems such as catheter migration, omental wrapping, constipation, and intraluminal obstruction with fibrin or clot; and it usually occurs shortly after initiation of peritoneal dialysis (PD).
What happens when you stop peritoneal dialysis?
Without dialysis, toxins build up in the blood, causing a condition called uremia. The patient will receive whatever medicines are necessary to manage symptoms of uremia and other medical conditions. Depending on how quickly the toxins build up, death usually follows anywhere from a few days to several weeks.