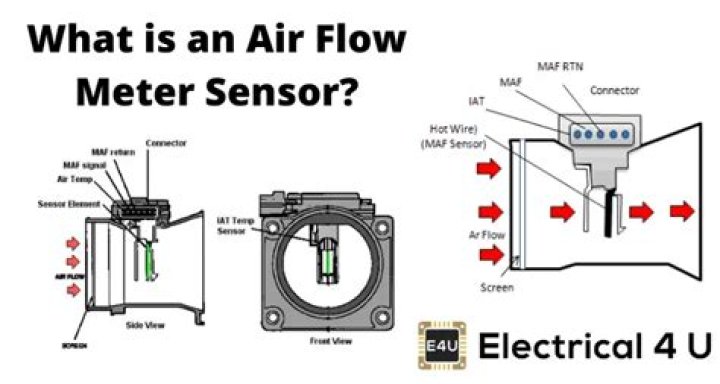
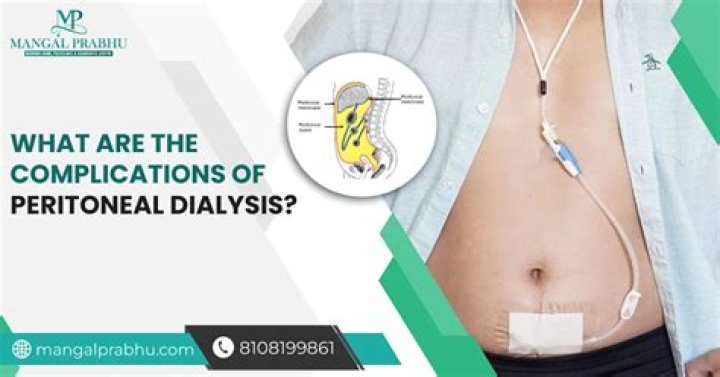
What are the complications of peritoneal dialysis
Infections. An infection of the abdominal lining (peritonitis) is a common complication of peritoneal dialysis. … Weight gain. The dialysate contains sugar (dextrose). … Hernia. Holding fluid in your abdomen for long periods may strain your muscles.Inadequate dialysis.
What is the most common complication in peritoneal dialysis?
The most frequent and important complication of peritoneal dialysis (PD) catheters is infection, which may result in catheter loss and discontinuation of PD [1,2].
What is a common problem with peritoneal dialysis?
Infections. The most common problem for people receiving peritoneal dialysis is peritonitis, an infection of the lining of the abdominal cavity (peritoneum). An infection can also develop at the site where the tube (catheter) is inserted to carry the cleansing fluid into and out of your abdomen.
What are the side effects of peritoneal dialysis?
The most common side effects of peritoneal dialysis include peritonitis, hernia, blood sugar changes, potassium imbalances, and weight gain. Report any symptoms you experience during treatment to your care team.How common is infection with peritoneal dialysis?
Peritoneal dialysis (PD) is associated with a high risk of infection of the peritoneum, subcutaneous tunnel and catheter exit site. Although quality standards demand an infection rate < 0.67 episodes/patient/year on dialysis, the reported overall rate of PD associated infection is 0.24-1.66 episodes/patient/year.
Which is a contraindication for use of peritoneal dialysis?
Clinical contraindications include inflammatory abdominal processes such as Crohn disease, ulcerative colitis, current clostridium difficile infection, and end-stage liver disease with ascites. The main anatomic contraindication to PD is an unrepaired hernia that would potentially increase in size with the use of PD.
What happens if too much fluid is removed during peritoneal dialysis?
Removing excessive fluid gain can make treatment uncomfortable. Patients can experience a sudden drop in blood pressure, which usually occurs toward the end of a dialysis treatment. You may feel nauseated, weak and tired because your body may not be used to having so much fluid removed at once.
What is the life expectancy of someone on peritoneal dialysis?
Median survival time was 20.4 months in patients receiving peritoneal dialysis versus 36.7 months in the hemodialysis group. At every age, patients with ESRD on dialysis have significantly increased mortality when compared with nondialysis patients and individuals without kidney disease.How do you know when a dialysis patient is dying?
Some of the most common end-of-life kidney failure signs include: Water retention/swelling of legs and feet. Loss of appetite, nausea, and vomiting. Confusion.
How do you know if your body is rejecting dialysis?In kidney failure some of you may have nausea, vomiting, a loss of appetite, weakness, increasing tiredness, itching, muscle cramps (especially in the legs) and anemia (a low blood count). With treatment for kidney failure, these symptoms will improve and you will begin to feel much better.
Article first time published onWhat happens when peritoneal dialysis stops working?
Without dialysis, toxins build up in the blood, causing a condition called uremia. The patient will receive whatever medicines are necessary to manage symptoms of uremia and other medical conditions. Depending on how quickly the toxins build up, death usually follows anywhere from a few days to several weeks.
What is the best position for peritoneal dialysis?
Placement of the peritoneal dialysis catheter requires that the patient be placed in a supine position.
What causes peritoneal dialysis to stop working?
The reasons for dropouts are multifactorial, that is, modality related, system related, and patient related. These include episodes of peritonitis, catheter-related problems, ultrafiltration failure, patient fatigue, and provider comfort.
What are the complications of peritonitis?
Complications of peritonitis include tertiary peritonitis, infection or dehiscence of the surgical site, enterocutaneous fistula, abdominal compartment syndrome, and enteric insufficiency.
What is secondary peritonitis?
Secondary bacterial peritonitis describes peritoneal infections secondary to intraabdominal lesions, such as perforation of the hollow viscus, bowel necrosis, nonbacterial peritonitis, or penetrating infectious processes.
How do I clean my peritoneal dialysis exit site?
- Clean your exit site.
- When showering, clean your exit site last using liquid antibacterial soap. …
- Rinse off the soap with water.
- Spray your exit site with vinegar solution.
- Pat dry with dry washcloth. …
- Secure your catheter with a small amount of slack to prevent pulling at the exit site.
Can you skip a day of peritoneal dialysis?
They either skip exchanges or sometimes skip entire treatment days when using CCPD. Skipping PD treatments has been shown to increase the risk of hospitalization and death.
Can kidneys start working again after dialysis?
The good news is that acute kidney failure can often be reversed. The kidneys usually start working again within several weeks to months after the underlying cause has been treated. Dialysis is needed until then.
Can dialysis remove water from lungs?
Hemodialysis can remove the excess fluid from the body in overhydrated patients, which in turn reduces water content of the lungs and thus decreases the pressure on airways, and reduces obstruction [27].
Who is not a candidate for peritoneal dialysis?
Identifying Patients There are only two absolute contra-indications for peritoneal dialysis: the absence of a functional peritoneal membrane and lack of a suitable home environment.
Is colostomy a contraindication to peritoneal dialysis?
BELIEF: Patients with an ostomy can’t do PD. FACT: Although there are concerns about leaks and catheter or exit site infection from urine or feces contamination, one study found reasonable outcomes for PD in patients with ostomies.
Why do you need peritoneal dialysis?
Why do I need peritoneal dialysis? You need treatment because your kidneys no longer clean enough wastes from your blood and remove extra fluid from your body. Even though people with kidney failure may still have some kidney function, it’s not enough and without treatment you will die.
What is the most common cause of death in dialysis patients?
Cardiovascular disease is the leading cause of death in dialysis patients and sudden death (SD) represents a significant proportion of overall mortality in both hemodialysis (HD) and peritoneal dialysis (PD) patients.
Why do dialysis patients turn dark?
Many reported cases of discolored skin, or hyperpigmentation, happen to people with ESRD. One cause of skin discoloration is related to pigments called urochromes being retained in the skin. Normally these are excreted by healthy kidneys. Patients with this condition tend to have a grayish, almost metallic color skin.
What organ shuts down first?
The brain is the first organ to begin to break down, and other organs follow suit. Living bacteria in the body, particularly in the bowels, play a major role in this decomposition process, or putrefaction.
How long can a 70 year old live on peritoneal dialysis?
Elderly patients on PD can attain favorable outcomes: the 2- and 5-year survival rates of patients over 65 years of age in Hong Kong were reported to be 88% and 56%, respectively 11. A study evaluating patients over 80 years of age reported a 12-month survival rate of 83% and a 24-month survival rate of 41%.
How long can a 70 year old live with Stage 4 kidney disease?
Stage 4 Kidney Disease: The kidneys are significantly damaged. Kidney failure becomes likely, which will require dialysis or a kidney transplant. A 40-year-old man with stage 4 kidney disease has a life expectancy of 14 years after diagnosis, while a 40-year-old woman can expect to live 16 more years.
Which is better PD or hemodialysis?
Compared with PD, hemodialysis (HD) has a higher dialysis efficacy and better capacity control, but a greater impact on hemodynamics and an increased tendency to bleed. At present, only one study has shown the effect of post-transplant dialysis modality in renal transplant recipients with DGF on 1-year outcomes.
What is the highest creatinine level before dialysis?
Creatinine levels that reach 2.0 or more in babies and 5.0 or more in adults may indicate severe kidney impairment. The need for a dialysis machine to remove wastes from the blood is based upon several considerations including the BUN, creatinine level, the potassium level and how much fluid the patient is retaining.
What happens when kidneys start to shut down?
If your kidneys stop working completely, your body fills with extra water and waste products. This condition is called uremia. Your hands or feet may swell. You will feel tired and weak because your body needs clean blood to function properly.
At what creatinine level should dialysis start?
National Kidney Foundation guidelines recommend you start dialysis when your kidney function drops to 15% or less — or if you have severe symptoms caused by your kidney disease, such as: shortness of breath, fatigue, muscle cramps, nausea or vomiting.