How do you repair a Cystocele
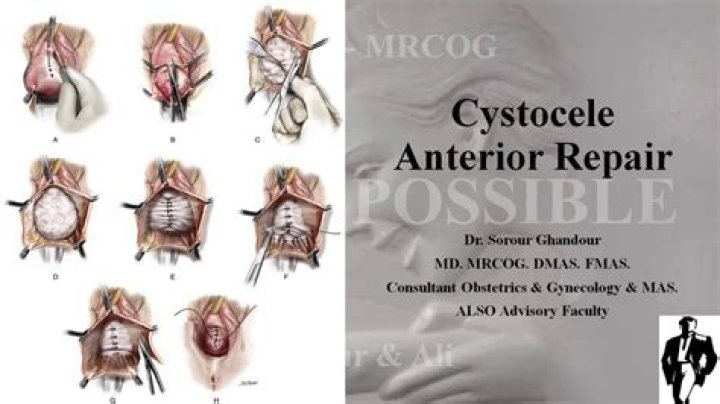
Under general anesthesia, an incision is made in the vaginal wall.The tissue between the bladder wall and the vaginal wall is tightened with stitches to allow the strengthening of the muscles and ligaments.
What is the best treatment for cystocele?
- Kegel exercises (pelvic floor strengthening exercises)
- Physical therapy.
- Vaginal pessary (a vaginal support device)
- Medications such as estrogen replacement therapy.
Can a cystocele correct itself?
Anterior prolapse is treatable. For a mild or moderate prolapse, nonsurgical treatment is often effective. In more severe cases, surgery may be necessary to keep the vagina and other pelvic organs in their proper positions.
How long is recovery from cystocele repair?
Women typically recover from the cystocele repair in about 4-6 weeks. Women typically recover from the cystocele repair in about 4-6 weeks. They may resume their daily activities, including sexual intercourse, in about 4 weeks after the procedure.Can cystocele be reversed?
Can Pelvic Prolapse be Reversed? Yes! Pelvic organ prolapse can be treated and improve without surgery in some women.
What does a cystocele feel like to touch?
Symptoms of cystocele include: Feeling of pelvic heaviness or fullness. Bulge in the vagina that you can feel. Aching or a feeling of pressure in the lower belly or pelvis.
How successful is cystocele surgery?
The anatomic success rate of cystocele repair was 75/79 (94.9%) and a highly significant improvement was noted for symptoms and on quality of life questionnaires.
How painful is prolapse surgery?
Usually the graft is anchored to the muscles of the pelvic floor. Generally this surgery is not very painful. You may feel as if you have been ‘riding on a horseback’. You will have some discomfort and pain, so please do not hesitate to take pain medication.How serious is Cystocele?
Although not life-threatening, a cystocele can have a negative impact on a woman’s quality of life. If it is not treated at all, the condition can continue to get worse. In the worst cases, the woman may be unable to urinate, which can cause kidney damage or infection.
Can you push a prolapsed bladder back into place?If you or your child has a rectal prolapse, you may be able to push the prolapse back into place as soon as it occurs. Your doctor will let you know if this is okay to do.
Article first time published onWhat kind of doctor does cystocele repair?
Your doctor may recommend a specialist with certification in Female Pelvic Medicine and Reproductive Surgery (FPMRS), such as a gynecologist, a urologist or a urogynecologist, also known as a urogyn. A urogynecologist is a medical doctor who has completed a residency in obstetrics and gynecology or urology.
What pessary is used for cystocele?
In patients with a mild cystocele, treatment using a ring with support, a dish with support, a Hodge with support or a donut pessary will suffice. To manage a large prolapse of the anterior vaginal wall, the Gellhorn pessary may be the best choice, although insertion and removal can be difficult.
Does a cystocele cause odor?
If you had a cystocele repair, the bladder catheter often needs to stay in longer—sometimes 2-6 days. This will allow the bladder more time to begin to work normally. You may notice an odor and/or bloody discharge from the vagina for 1-2 weeks.
Does Grade 2 Cystocele require surgery?
Grade 2 Cystocele This type of cystocele causes major discomfort and severe urinary incontinence. The treatment for this type of cystocele is usually some form of cystocele repair surgery but the cystocele may also be treated with a pessary device.
Is walking good for bladder prolapse?
walking – this is the best exercise during bladder prolapse surgery recovery. doing pelvic floor exercises. resting each day.
Is Cystocele a cause of urinary tract infections?
Defects at any of these levels, and usually a combination of two or all three of them, result in typical anterior compartment prolapse (cystocele), which may predispose to UTIs.
Is prolapse surgery a major surgery?
Vaginal prolapse surgery is a major surgery with serious risks and potential complications. You may have less invasive treatment options depending on your circumstances.
What can be used instead of mesh for prolapse?
There are a number of nonsurgical options that can address pelvic organ prolapse and stress incontinence, including physical therapy to strengthen the pelvic floor and devices called pessaries that are made of silicone and can be placed into the vagina to hold the organs in place.
How long do you stay in hospital after prolapse surgery?
You’ll usually need to stay in hospital overnight or for a few days. Most women can go home once their bladder is emptying well. In rare cases, you may need a catheter for a week or so. You’ll still be able to go home, but you’ll need to come back in a week or two to have the catheter removed.
How do you know if your bladder has fallen?
Patients can usually tell if their bladder has dropped when they face difficulty urinating, pain or discomfort, and stress incontinence (leakage of urine due to exertion or coughing, sneezing, and laughing), which are the most common symptoms of a prolapsed bladder.
How do you drain a bladder with a prolapse?
- Empty when you sense the appropriate urge.
- Bulge your abdomen forwards and make your waist wide as you empty.
- Relax your pelvic floor muscles.
- Breathe normally.
- Take your time.
Can a woman's bladder fall out?
Under normal conditions in women, the bladder is held in place by a “hammock” of supportive pelvic floor muscles and tissue. When these tissues are stretched and/or become weak, the bladder can drop and bulge through this layer and into the vagina. This results in bladder prolapse, also called cystocele.
Does Cystocele cause stress incontinence?
Anterior vaginal wall prolapse may present as stress incontinence. A large cystocele may cause urethral kinking and overflow incontinence.
What is the best surgery for prolapsed bladder?
A healthcare provider may recommend surgery to repair the vaginal wall support and reposition the woman’s bladder to its normal position. The most common prolapsed bladder repair is an anterior vaginal repair—or anterior colporrhaphy.
How many hours is prolapse surgery?
The length of operative time for laparoscopic colposuspension can vary greatly (3-5 hours) from patient to patient depending on the internal anatomy, shape of the pelvis, weight of the patient, and presence of scarring or inflammation in the pelvis due to infection or prior abdominal/pelvic surgery.
What is the success rate of bladder prolapse surgery?
Approximately 94% achieved surgical success when it was defined as the absence of prolapse beyond the hymen. Subjective cure (absence of bulge symptoms) occurred in 92.1% while absence of re-treatment occurred in 97.2% of participants.
When should you have surgery for prolapse?
Consider surgery if the prolapse is causing pain, if you are having problems with your bladder and bowels, or if the prolapse is making it hard for you to do activities you enjoy. An organ can prolapse again after surgery. Surgery in one part of your pelvis can make a prolapse in another part worse.
How do you fix a prolapsed bladder without surgery?
The two non-surgical options for prolapse are pelvic floor muscle training (PFMT) and a vaginal pessary. PFMT can be effective for mild prolapse but is usually not successful for moderate and advanced prolapse. The main alternative to surgery for prolapse is a vaginal pessary.
Does a urologist treat prolapsed bladder?
Urologists may treat UTIs, incontinence, cancer, and male infertility problems, among other conditions. Urogynecologists see women and focus on symptoms related to urinary incontinence, prolapse, and pelvic floor disorders.
How can a dr tell if you have a prolapsed bladder?
An exam of the female genitalia and pelvis, known as a pelvic exam, is required in order to diagnose a prolapsed bladder. A bladder that has entered the vagina confirms the diagnosis. For less obvious cases, the doctor may use a voiding cystourethrogram to help with the diagnosis.
How long does it take to recover from bladder surgery?
After leaving the hospital, the person should expect to take several weeks for recovery. During this time, their body is healing from the surgery, so they should only perform light activities. After 4–6 weeks, doctors will usually allow a person who has had their bladder removed to resume normal activities.