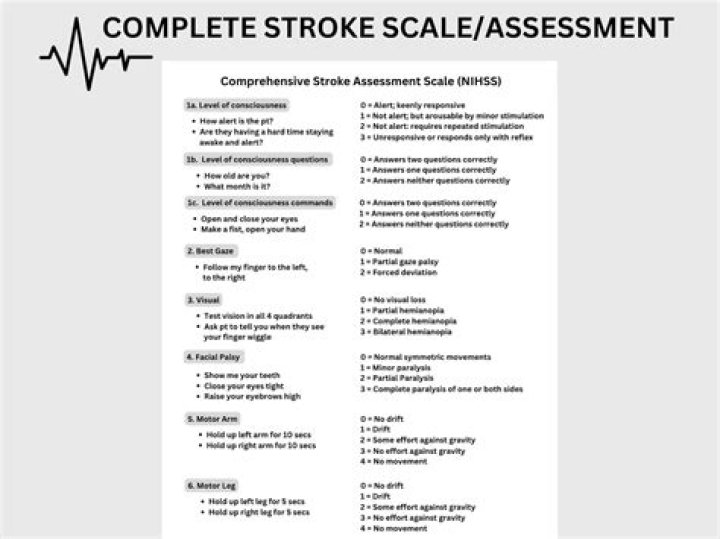
Does Self Etch remove smear layer
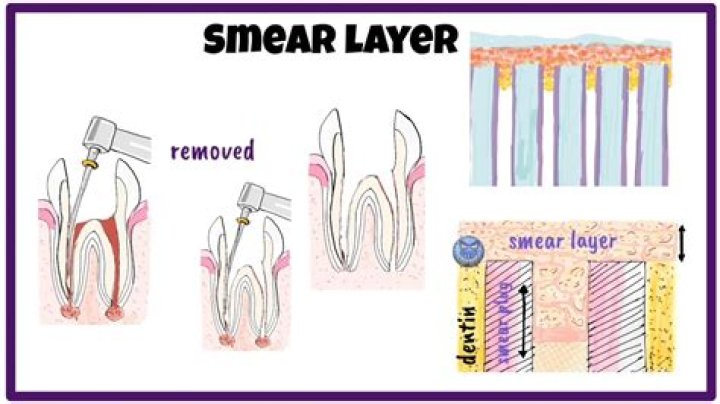
Self-etch adhesives: They include an acidic monomer that simultaneously demineralizes and penetrates into the dentin surface, making the smear layer permeable without removing it completely.
Does etch remove smear layer?
The purpose of etching is to remove the smear layer that is present after tooth preparation. In addition it opens the dentinal tubules, demineralizing enough of the dentin to allow the formation of resin tags within the dentin structure.
What happens to the smear layer when applying a self-etch adhesive?
When phosphoric acid is applied to dentin, the smear layer is converted to a liquid form prior to rinsing with water. When using a self-etch primer, the smear layer is dissolved into the primer, and becomes one. Air-drying is done instead of rinsing.
How do you remove a smear layer?
There are three main methods to remove smear layer: chemically, mechanically (ultrasonically), laser, or combinations. No one single irrigant has the ability to kill microorganisms, dissolve organic tissues, and demineralize smear layer.Which material removes the smear layer during restorative process?
Most commonly, a neutral solution of ethylene diamine tetra-acetic acid is used for removing the smear layer in the root canal [ 51 , 52 ].
What is Self-etch?
Self-etch adhesives contain acidic monomers, which etch and prime the tooth simultaneously. Etch-and-rinse adhesives are offered as two- or three-step systems, depending on whether primer and bonding are separate or combined in a single bottle. Similarly, self-etch adhesives are available as one- or two-step systems.
Which is better self-etch or total-etch?
Self-etch and selective-etch are the most predictable relative to production of postoperative tooth sensitivity. Total-etch can cause more postoperative sensitivity if not done well. If you are currently successful with the technique you’re using, don’t change.
Should smear layer be removed?
Removing the smear layer allows for more cleaning and disinfecting root canal walls and better adaptation of root canal filling materials. However, the presence of smear layer can act as a seal to the dentinal tubules and minimize the ability of bacteria and its toxins from penetrating the dentinal tubules.Does sodium hypochlorite remove smear layer?
The two sodium hypochlorite solutions did not remove the smear layer, even when 5% sodium hypochlorite was scrubbed on the dentinal walls. … The other three solutions effectively removed the smear layer, but no significant difference was found between them (p > 0.05).
Which of the following removes the smear layer from the walls of the root canal?Chelating agents are effective in that they remove the smear layer, open the dentinal tubules, and produce a clean surface for closer obturation. Removal of the smear layer encourages the creation of a good apical plug to prevent over filling, post-filling sensitivity, and possible microleakage.
Article first time published onWhy is the smear layer important?
The smear layer can affect bonding, disinfection as well as obturation hence why it is considered important to remove. … Impaired obturation Following mechanical tooth preparation during endodontic procedures the smear layer can act as a barrier between filling materials and the root canal wall.
What is smear plug?
(smēr plŭg) Plugs of grinding debris that extend 1-5 mcm into dentin tubules.
How long is the etchant material applied to the tooth being prepared for use of a bonding material?
The preparation should be etched for 15 to 20 seconds with an acid gel. The etchant should extend well beyond the cavosurface margin to cover any susceptible pits and fissures not included in the preparation. After thoroughly rinsing the etch from the tooth, a dentin-bonding agent is applied and cured.
What does the smear layer consists of?
The smear layer, comprising both organic and inorganic components, is found on the root canal walls after endodontic instrumentation. It is composed largely of particulate dentine debris created by endodontic instruments during root canal preparation but also contains pulpal remnants and microorganisms.
What is the smear layer made of?
When the root canals are instrumented during endodontic therapy, a layer of material composed of dentine, remnants of pulp tissue and odontoblastic processes, and sometimes bacteria, is always formed on the canal walls. This layer has been called the smear layer.
What is EDTA in dentistry?
EDTA works by reacting with the mineral components of the hard tissues of the tooth. The chelating agent EDTA softens the tissues, decalcifying the canal walls. It facilitates the mechanical preparation of the root canal and further removal of the smear layer, which opens dentin tubules.
How long should you etch primary teeth?
45~60 seconds was the optimal time for etching on the primary enamel.
What does self etching primer do?
What Is Self Etching Primer? Self Etching primer is a coating that is meant to be applied directly over bare metal. … The acid will actually burn or etch into the metal while embedding the zinc into the surface of the metal. This ensures good adhesion and rust prevention.
Does tooth etching damage enamel?
The process of etching in the tooth surface leads to demineralization of enamel in tooth. This leads to increase in porosity in tooth; this can aid in more water deposition on the surface.
Do you sand self etching primer?
In any complete restoration or body repair project, you will to sand primer at one point or another. However, most manufacturers of self-etching primer, due to the acid base of the products, don’t recommend directly sanding the self-etching primer.
What is self etching primer dentistry?
In conservative dentistry, self-etching primers are being increasingly used in place of phosphoric acid etching for composite resin restorations, and their efficacy with respect to adhesion to dentin and enamel has been reported. 6–9 Self-etching primers function both as an etching agent and a primer.
What does etching do to enamel?
Acid etching is the use of an acidic substance to prepare the tooth’s natural enamel for the application of an adhesive. The acid roughens the surface microscopically, increasing retention of resin sealant. Etching of dental enamel with acid removes the smear layer and opens enamel tubules.
Does EDTA remove smear layer?
The results show that the smear layer can be totally removed by using 10 ml of a four-to-three by volume mixture of EDTA and ethylenediamine for irrigation of instrumented root canals.
How do you dilute sodium hypochlorite for Endo?
It is recommended to begin with a 5.35% concentration of sodium hypochlorite. With a 1:1 dilution, a 2.5% (w/v) concentration might be obtained, that is to say, use one part of 5.25% sodium hypochlorite with the same volume of water to arrive at the desired result.
Does enamel have a smear layer?
Smear layers were thicker on enamel than on dentin, irrespective of the finishing methods used. Therefore, different thicknesses of smear layer on enamel/dentin might be an important factor to consider when evaluating the bonding efficacy of self-etching adhesives to both tooth substrates.
What is hybrid layer in dentistry?
The layer of dentine which has been conditioned to remove the loosely adherent smear layer and into which adhesive resin has flowed to form a collagen/resin phase. … Hybrid layer as a dentin-bonding mechanism. Journal of Esthetic Dentistry 1991;3:133–8.
When an endodontists obturate a canal What are they doing?
The clinical goal of endodontic obturation of a root-canal system is to fill empty spaces, promote hermetic sealing, and prevent bacterial activity from infiltrating the periapical tissues.
What is the endodontic biofilm?
Endodontic disease is a biofilm-mediated infection, and primary aim in the management of endodontic disease is the elimination of bacterial biofilm from the root canal system. The most common endodontic infection is caused by the surface-associated growth of microorganisms.
What is remaining dentine thickness?
Previous studies have suggested a remaining dentine thickness of 2 mm for protection of the pulp,17 others suggest 1 mm18 but a minimum of 0.5 mm is now accepted. 8 When the lesion reaches within 0.25 mm-0.3 mm of the pulp, inflammatory reactions of pulpitis and hyperaemia are initiated.
Why are retention pins used in complex restoration?
Later, several types of pins became popular retentive devices in complex amalgam restorations. In recent years, the emphasis has shifted from creating adequate retention form to providing adequate resistance form to prevent restoration displacement, restoration fracture, or fracture of remain ing tooth structure.
How and why dentin sealers are used in the restoration process?
- Seals dentinal tubules.
- Reduces microleakage around a restoration.
- Acts as a barrier to protect the tooth from highly acidic base or cements such as zinc phosphate.